Abstract
Background: There are ongoing concerns regarding adherence to contact lens (CL) care regimens by wearers. Global studies evaluating behavioural trends have shown that full compliance to CL wear is rare and widespread non-compliance exists.
Aim: This study aimed to identify levels of compliance with recommended care regimens by probing the attitudes and behaviours of soft CL wearers.
Setting: Gauteng, South Africa
Methods: A cross-sectional design was used to pose questionnaires to CL wearers and optometrists. Data were collected quantitatively via convenience sampling.
Results: A total of (n = 171) CL participants responded, with more female (63%) than male (37%) wearers. Two-thirds (66%) used monthly lenses and (59%) knew when it was time to replace lenses. Of those, 72% did not know which brand of CLs they wore, while 74% were unsure of which multipurpose solution was used. Low levels of case hygiene were found with close to half (48%) never cleaning or disinfecting CL cases. It emerged that 77% of participants reported having received instruction from an optometrist on CL care; however, non-adherence was evident.
Data collected from (n = 125) participant optometrists showed that less than half (45%), rated patients as having average compliance despite 61% of CL wearers on the contrary expressing satisfaction with care regimens.
Conclusion: Results provide evidence that suggests a cause for concern in many areas related to compliance by CL wearers.
Contribution: Optometrists and CL wearers were investigated thus providing insight into CL wear habits from two perspectives.
Keywords: contact lenses; eye health; vision correction; compliance; contact lens care regimen.
Introduction
Contact lenses (CLs) are a widely accepted modality for refractive error correction and cosmetic enhancement but a lack of proper compliance with CL care regimens is widespread.1 Most CL wearers enjoy various advantages including improved cosmesis, a wider field of view, vision enhancement because of the absence of reflections, avoidance of spectacle lens fogging and more stable vision, where refractive error between the two eyes differs significantly.2 Although many have been successful wearers for several years, there seems to be an abandonment of CL wear eventually, or reduced usage to occasional rather than daily wear as eyes can become intolerant to CLs.3 Intolerance is prevalent among CL users who have not followed recommended guidelines; to name a few examples: failure to replace lenses timeously, and wearing soiled lenses leading to redness or dryness of eyes, which can cause irreversible changes in eye tissues.4 In addition, poor hand and case hygiene practise, not replacing case solution daily, overnight wear of lenses, using water instead of a multipurpose solution, wearing lenses for excessive periods, and eye infections are all causative factors for CL use dropouts and increased risk of infection.2
Optometrists are aware that CL use increases eye infection risks; however, millions of patients worldwide are fitted with CLs because this risk is manageable.5 A significant risk factor in patient non-compliance with recommended hygienic practice is contracting microbial keratitis, a severe complication that is potentially sight-threatening.6 Wearing CLs increases the risk of infection, as they are foreign bodies placed on the eye that interfere with the efficient tear exchange system occurring with the sweeping action of the lids. Contact lenses provide a surface onto which bacteria may adhere and biofilms form on the lens surface. Lenses in turn protect bacteria from being exposed to corneal defence mechanisms. As a result, epithelial antimicrobial defences are inhibited, and pro-inflammatory mediators compromise epithelial barrier function.6
Responsibility for compliance is shared between optometrist and patient. It is an optometrist’s responsibility to provide a patient with all the information regarding CL use including hand hygiene, wear schedules, cleaning, handling, storage, disposal and annual examination.7 Thereafter, it becomes the patient’s responsibility to adhere to instructions.8 Although prescribing optometrists are governed by strict rules in dispensing CLs, there appears to still be low rates of compliance among CL wearers globally.
Methods
Data were collected from CL wearers using semi-structured, self-administered online questionnaires. Optometric participants who consented answered a questionnaire from an article posted by Vision Online, a monthly electronic magazine (e-magazine) distributed to optometrists. Optometrists who were aware of the study invited CL wearers by providing a link that directed them to Vision Online’s CL wearer questionnaire. Respondents were informed that participation was voluntary, and they had a right to withdraw without risk of penalty or prejudicial treatment. For anonymity, no names were recorded on questionnaires and no monetary reward was offered. Website survey design ensured that no edits could be made to responses by the researcher, and participants’ online data were kept safe as no personal details were recorded. They were also informed that the benefits of data collected in this study using questionnaires might be a valuable addition in contributing towards enhancing appreciation of areas needing improvement in CL wearers’ care regimens.
Questions posed to CL wearers were structured in alignment with the research aim and objectives and included the following: demographics; the ability of participants to identify the brand of CLs and solutions they use; whether or not instructions by an optometrist on how to use CLs were provided; how long they had been wearing CLs; knowledge of recommended care practises, such as frequency of CL case and solution replacement and what prompted the participant to replace CLs. Habits such as hand washing before handling, use of CLs while swimming and showering, method of storage and case cleaning were also surveyed. Other behavioural tendencies, such as how often CL cases were disinfected, were queried, and an open-ended question on how participants could improve compliance was probed to gain better insight into behavioural trends.
Only soft CL wearers residing in Gauteng province were invited to participate and respondents who provided consent to participate were included. Age category 18–65 years was used, as other studies have shown the mean age range of CL wearers to be in this category.9 Females and males were included.
Cochran’s formula was used to calculate ideal sample size based on the desired level of precision, confidence level and estimated proportion of the population, which has the attribute in question.10 The formula used is as follows:
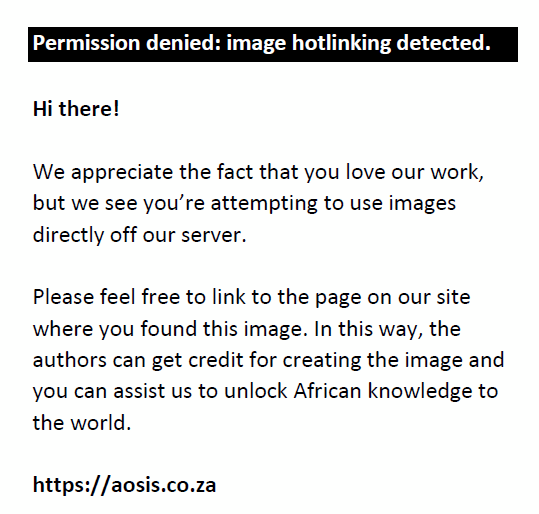
where nO is the estimated sample size, e is the desired level of precision (or margin of error), p is the estimated proportion of the population with the attribute in question, q = 1 – p and Z corresponds to the level of confidence required. Applying the given formula, based on a desired margin of error of 5%, desired 95% confidence level, and corresponding Z value of 1.96 as found in the z table, the ideal sample size was 384 CL wearers. However, the given formula assumed a large to infinite proportion of CL wearers within the targeted geographic area. Calculation was therefore modified to cater for a smaller estimated population of 1000 CL wearers in Gauteng. This was performed using following Cochran’s finite population correction formula11:
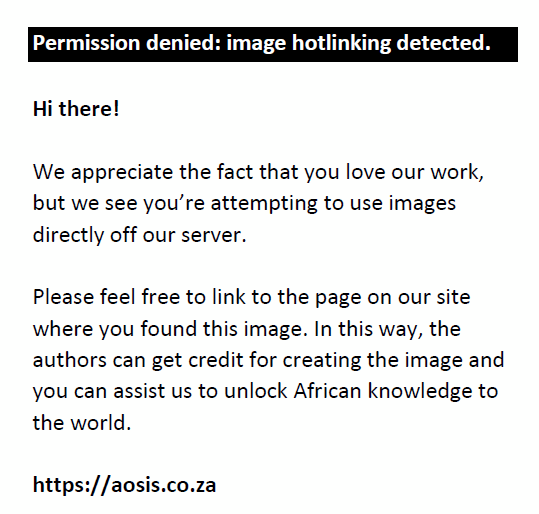
where nO is the Cochran’s formula sample size recommendation (here 384) with N the estimated target population size (i.e., 1000) and n is the new adjusted sample size.
Thus, the final required sample size obtained from the given calculation was 278. However, because of a combination of unforseen logistical, budgetary and time limitations, only 171 soft CL wearers eventually completed the survey. This increased the resultant margin of error from initially desired 5% – 7% at the 95% confidence level but this was considered acceptable. There is nothing sacrosanct when setting confidence levels, and even a margin of error of 10% is acceptable, especially where purpose is to deduce trends or infer results in an exploratory manner.12
Pre-study pilot testing is useful to achieve the following: detect errors and ambiguity in questions; ensure that individuals understand questionnaire content in the manner intended by researchers and recognise problems related to layout and presentation, which could potentially lead to misunderstanding of questions.13 The researcher administered the pilot survey by convenience sampling to 10 optometrists in attendance at a conference who treated CL patients’ and understood the rationale behind the questionnaire content. After completion of consent form and questionnaires, a focus group discussion was held, and all 10 optometrists gave their views on the relevance of questions, ease of understanding, time taken to complete and whether questions would address the study objectives. Suggested edits were made to both questionnaires, prior to participant presentation.
Thereafter, permission was sought from optometrists seeing CL wearers in Gauteng, to invite their patients to complete questionnaires via an article posted by Vision Online, a monthly electronic magazine (e-magazine) distributed to optometrists. Optometrists in Gauteng, who agreed to participate, received a link, and sent it on to CL wearers in their patient databases. All study participants were requested to read the information letter, which explained why research was being carried out, how it was to be performed, as well as time it would take to complete, which averaged between 8 and 10 min for CL participants and 5 min for optometrist participants in the pilot study. Survey results were further protected from bias as Internet Protocol (IP) addresses were recognised and this ensured that no participant could respond multiple times. Online surveys were active online for a period of 6 months and thereafter, responses were captured into Microsoft Excel format, by the researcher to begin statistical analysis.
Data analysis
Data collected were analysed using IBM® Statistical Package for the Social Sciences (SPSS, version 22). Descriptive statistics that reflected basic features of data in other studies were applied to present the study sample profile and to describe attitudes and behaviour of soft CL wearers.14 Results of the descriptive analysis were presented in frequencies and percentages for categorical variables and in means and standard deviations for continuous variables.
Normality of data distribution was examined using the skewness statistic, which is a measure of asymmetry in variable distribution.15 Skewness was tested for data concerning gender, education, employment status and number of years of CL wear. The skewness values for all these variables were equal to or less than 0.5 and thus indicated sufficiently normal sample data distributions.15 As a result, parametric statistical methods were suitable for subsequent multivariate analysis. The Chi-square test of association is designed to analyse group differences when a dependent variable is measured at a nominal level.16 This test was used to compare attitudes and behaviours of soft CL wearers according to demographics. One-way analysis of variance (ANOVA) determines group mean differences by using between- and within-group variance differences.17 This was used for comparisons of variables measured on continuous and categorial scales.
With respect to optometrists, and given the small population, the approach was to target all optometrists in the Gauteng Province. Therefore, a prior ideal sample size calculation was not necessary for this target group. In South Africa, there are 3800 registered optometrists of which 2600 are practising, and of these, 46% work in Gauteng.18 Vision Online has 2800 optometrists registered on their database. A total of 125 optometrists responded. Questions presented to optometrists included: demographics, enquiring how optometrists rated overall compliance of CL wearers to recommended care and wear regimens; if CL cost was perceived as a factor to non-compliance and input on the most commonly observed pathologies. Open-ended questions were also presented, giving optometrists’ an opportunity to provide suggestions as to how compliance could be improved.
Data were analysed using IBM® SPSS. Descriptive statistics presenting study sample profiles and describing optometrists’ practices and perceptions about soft CL wearers were used in collecting data analysis.
This study encompasses two participant populations: CL wearers and optometrists and they are discussed separately in the next section.
Results of contact lens participants
A total 171 soft CL wearers participated in the study and of these 107 (63%) were female and 64 (37%) were male as shown in Figure 1.
 |
FIGURE 1: Gender of soft contact lens wearer participants (N = 171). |
|
Age groups
As displayed in Figure 2, more than a third (36%) of CL participants were aged between 18 and 30 years, 34% were in 31–40 years age range and 30% were older than 40 years. Mean age was not calculated as age ranges were probed, and not specific ages.
 |
FIGURE 2: Age groups of contact lens participants (N = 171). |
|
Education
Figure 3 depicts education levels obtained. About a quarter (26%) of CL participants were educated up to high school level, approximately half (52%) held bachelors’ degrees, 15% held masters’ degrees and 5% held a doctorate.
 |
FIGURE 3: Highest level of education achieved (N = 171). |
|
Employment
Employment status is shown in Figure 4. A majority (42%) of CL participants were employed full time, 20% part time, 23% self-employed and 15% were unemployed.
Two-thirds (66%) of CL participants used monthly lenses while much lower percentages of 19% used dailies and 13% used biweekly lenses. A small percentage (2%) were unsure about type of lens they used. When probed more closely on which brand CL participants used, majority (72%) could not identify the brand they wore and a large proportion (74%) were unsure of the brand of CL multipurpose solution they used.
Most participants in this study were experienced CL wearers; one-fifth (20%) reportedly wore CLs for up to 12 months, about a quarter (26%) for between 1 and 5 years, (22%) for 5–10 years and about a third (32%) for more than 10 years.
The questionnaire CL participants completed probed on hygiene-related risk behaviours, namely frequency of CL case change and consistent replacement of CL case solution. Approximately 53% of participants reported changing their CL cases with each new bottle of multipurpose solution opened and 47% did not do so. Two-thirds (66%) of participants used fresh CL solution daily. Approximately a third (34%) of CL wearers showed low compliance with case hygiene regimen and did not discard solution in the case daily. A third (33%) of participants never slept with CLs in situ, 29% seldom did so and 26% did so occasionally, while at least 12% slept with CLs in situ almost all the time. Although the frequency of sleeping with CLs inserted was generally low, it was significantly higher among the unemployed than the self-employed (p = 0.01). Frequency of handwashing before inserting and removing CLs from the eyes was generally high at 80%. Use of CLs in situ while showering or swimming was also probed, and it emerged that 47% of participants seldom or never swam or showered while wearing CLs; 43% did so occasionally and 10% every time or close to all the time. Contact lens participants were asked open-ended questions on how they could change behaviour to achieve better compliance, responses of which are indicated in Table 1.
| TABLE 1: Contact lens participant responses on how they believe compliance could be improved (N = 171). |
Attitudes
Most participants (72%) did not find it necessary to know the brand of CLs they were wearing. In addition, a large proportion (74%) of CL participants reported being unsure of which CL solution they used. When probed on the effect of cost on timeous CL replacement; 61% reported that CL cost affected the decision on when to replace lenses, while 27% reported cost did not affect the decision and 12% were neutral. Contrarily, 82% of optometrists reported cost to be a moderate to major barrier to CL wearers not replacing lenses timeously. Contact lens participants older than 50 years considered CL cost in decisions on when to replace lenses significantly more than the younger age groups (p = 0.02). The unemployed also considered CL cost when deciding on when to replace lenses significantly more than full-time employed and self-employed participants (p = 0.01).
Just over half (52%) of CL participants in this study felt it was necessary to have a pair of current prescription spectacles. Therefore, there is a possibility that close to half of CL wearers in this study overwear lenses as they are not in possession of updated spectacles. Interestingly, of the 171 CL participants in this study, 77% confirmed that an optometrist provided them with instructions on the CLs care regimen, while 23% reported never having received instructions.
Table 2 shows responses from CL wearers when probed on what behavioural measures they took in adhering to timeous replacement of CLs.
| TABLE 2: How contact lens wearers decide on when it is time to replace contact lens (N = 171). |
Fifty-four percent (n = 94) of CL participants reported having had eye infections, and of those, 43% said CLs were sometimes the causative factor, while 28% reported that CLs were seldomly the cause. This finding was contrary to other research performed in Africa by Gwata, where a mere 8% of CL wearers reported eye infections.19
Results of optometrist participants
A total of 125 optometrist participants completed the questionnaire; of these 85 (68%) were female and 40 (32%) were male as shown in Figure 5.
 |
FIGURE 5: Gender distribution of participants. |
|
Age groups
Most optometrist participants who responded (44%) were in age category 31–40 years. In age category 41–50, there were 24%; between ages 18–30 and > 50 categories, there were 16% of optometrists in each. These results are shown in Figure 6.
Education
A majority of optometrist participants (79%) held a bachelor’s qualification, and only 12% proceeded to obtain a postgraduate degree. Nine percent of optometrists were in possession of diplomas (Figure 7).
 |
FIGURE 7: Education distribution of participants. |
|
Optometrists reported the following attitudes and behaviours of CL wearers (refer to Table 3) they observed on average, weekly.
| TABLE 3: Number of patients attended to weekly by optometrists with the following negative attitudes and behaviours (N = 125). |
Of concern is that 19% of CL wearers were unaware of complications that could arise from improper CL use and 12% did not have back up current spectacles, which could lead to over wear of CLs. It was evident that optometrists reported just under 10% of participants overwearing lenses. On the contrary, it was pleasing to observe that at least 22% of CL wearers did not display any of the negative behaviours listed in Table 3. Optometrists were asked open-ended questions on how they suggest compliance of soft CL wearers could be improved and their responses are outlined in Table 4.
| TABLE 4: Distribution of suggestions from optometrists on improving contact lenses compliance. |
A majority of optometrist participants (45%) felt that educating patients and providing them with written instructions could contribute to better compliance.
Discussion
This study targeted both CL wearers’ and optometrists’ in an attempt to investigate the attitudes and behaviour of CL wearers in Gauteng. More female (63%) than male (37%) CL wearers participated in this study, indicating that more female CL wearers were willing to complete surveys than males, consistent with findings of studies conducted by Morgan et al.,9 and Makrynioti et al.19 In addition, most CL participants were educated and employed, which is in line with conclusions of an American population-based survey on 40.9 million people, where majority of CL wearers were found to be young, female and more educated Cope et al.20
A majority (70%) of CL participants in this study fell within age range of 18–40 years, in alignment with mean ages of participants in other studies conducted in Africa by Gwata21 and Khoza et al.22 where participants were found to be in a similar range with a mean age of 33 years. This study further highlighted a lower number of wearers in age category 41–50 years, where 18% of wearers were observed and even fewer wearers in age range 50 years and above at 12%.
A majority (66%) of (N = 171) soft CL participants in this study reported using monthly CL; consistent with findings in other studies performed by Bakkar et al.,23 and Morgan et al.1 However, this is contrary to findings of research conducted by Rueff et al.,24 in which majority, (46%) of CL participants were on bi-weekly lenses, 34% on monthlies, and 20% on dailies. It appears that lens types with highest number of wearers differ across continents, and therefore, behavioural traits would be expected to vary globally. Although daily CLs are superior for corneal health and provide simpler care processes as there are no steps involved in lens cleaning, they are more expensive. Thus, cost implications could be one of the major factors in monthly lenses being more popular.
The responses collected and analysed from participants in this study were on CL hygiene-related risk behaviours, namely the washing of hands before handling CLs, frequency of CL case change, and consistent replacement of CL case solutions when storing CLs. High compliance rates (80%) with hand hygiene regimens were reported, aligned with findings of the studies conducted by Wu et al.25 and Khoza et al.22 This study commenced before the coronavirus disease 2019 (COVID-19) pandemic, which drove aggressive global awareness campaigns towards frequent handwashing prior to touching the face. Therefore, if pleasing results were identified at that stage, compliance is likely to remain high because of elevated awareness of the importance of rigorous hand hygiene post-COVID-19.
On the contrary, of particular concern were 47% of CL wearers who reported not changing their CL cases with each new bottle of multipurpose solution opened. Infrequent replacement of CL cases was found to be associated with serious eye infections and discomfort. Repeated poor handling of the lens and case as reported in this study by 34% of the participants affords opportunities for the introduction of microorganisms, while the moist surface of the lens and case creates an environment conducive to microbial growth.1,23,25
More emphasis by South African optometrists should be placed on CL case hygiene, avoidance of using water with CLs and timeous replacement of CLs. These behavioural practises have the potential to cause sight-threatening microbial infections as the same tendencies to non-compliance have been observed in other studies.1,23,25 Optometrist participants further reported that approximately two CL wearers per week expressed unhappiness over costs related to CLs. As cost factors most likely impact decisions by CL wearers to replace lenses timeously, this situation could be even more frustrating for unemployed CL wearers, leading to use of other means to clean lenses, such as tap water; and non-compliance with timeous lens replacement. In addition, as reported by optometrist participants, costs could also be a contributing factor to most reported top four pathologies: dry eyes were indicated by 32% of optometrists, blepharo-conjunctivitis by 16%, giant papillary conjunctivitis (GPC) by 8% and corneal neovascularisation also by 8% of optometrists. There may be cause for concern as more than half of CL participants in Gauteng reported experiencing previous eye infections in this study. Optometrists should identify high-risk CL wearers, and suggest 6 monthly evaluations for those known to default.
Limitations of the study
There was a lower uptake rate by participants than anticipated, and this could be attributed to CL wearers not being aware of the study, or not wishing to complete a questionnaire because of time constraints. Therefore, the sample may not represent all soft CL wearers in Gauteng; however, it provides a baseline. South Africa has 11 official languages, and Gauteng has a large majority of mixed heritages. The questionnaire in this research was designed only in English. As a result of most participants not being aware of which brand of CLs they used, it cannot be deduced with certainty whether participants who slept while wearing CLs did so correctly or not as this study did not further probe if lenses worn were originally prescribed as extended wear lenses. In addition, there was evidence of higher incidence of CL wearers reporting previous infections. Whether or not related to CL wear, this study did not probe in-depth questioning on infection symptoms and thus it is unknown if participants may have reported ocular allergies, dry eyes or another form of visual discomfort as being infection. Future studies could investigate the cause of eye irritations or infection anomalies further, by asking more precise questions to CL wearers to enable distinction.
Conclusion
The study identified the need to place emphasis on several categories as a cause for concern has been notably found in these areas.
Optometrist involvement
It should be ensured that education is provided at each visit by eye care practitioners regarding the correct wear regime including; detailing replacement protocols for the specific lens worn, cleaning, storing and discarding CL solution and cases. Strict adherence to Health Professions Council of South Africa (HPCSA) recommendations, which state that CLs should only be dispensed if the wearer has had a visual examination not exceeding 12 months, should be exercised by all optometrists’.
Behavioural
Good CL-related behaviour should be encouraged and wearers should abstain from the use of water while using CLs; this refers to showering, swimming, bathing or cleaning CLs with water. In addition, CL wearers should be educated to discard disinfecting solutions in the case of daily, use prescribed appropriate multipurpose solutions, and replace cases quarterly to avoid eye infections. The CLs should not be slept with unless specifically prescribed for that purpose.
Attitude
Prevention is better than cure, and therefore, at each visit, eye care practitioners should continuously strive to promote awareness of CL-related complications because some of which are sight-threatening. With this approach, attitudes and behaviour could change when CL wearers realise the need for compliance to reduce risks. This may lead to an improvement in CL-related complications, fewer cases of dropout and lower levels of frustration for both CL wearer and eye care practitioner.
Acknowledgements
The authors would like to acknowledge Vision Online e-magazine and Khumbula consulting.
Competing interests
The authors declare that they have no financial or personal relationships that may have inappropriately influenced them in writing this article.
Authors’ contributions
This research forms part and is partially based on the MPhil dissertation, The attitudes and behaviour of soft contact lens wearers towards compliance concerning their care regimen in Gauteng (South Africa) (https://hdl.handle.net/10210/498800), undertaken by T.B.N., who conceived the original idea at the UJ. The research was supervised by T.I.M. and D.B..
Ethical considerations
Ethical clearance was granted by the Faculty of Health Science Research Ethics Committee (REC) at the UJ before the study commenced, and it was renewed annually until completion of the study. An ethical clearance certificate REC-01-191-2019 and Higher Degrees Committee (HDC) clearance HDC-01-127-2018 was obtained.
Funding information
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Data availability
Data supporting the findings of this study are available from the corresponding author, T.B.N, on request.
Disclaimer
Views and opinions are expressed by the author and do not necessarily reflect the official policy of the institution.
References
- Morgan P. Contact lens compliance and reducing the risk of keratitis. Optician. 2007;234(6109):20–25.
- McMonnies CW. Improving contact lens compliance by explaining the benefits of compliant procedures. Cont Lens Anterior Eye. 2011;34(5):249–252. https://doi.org/10.1016/j.clae.2011.06.006
- Lim C, Carnt N, Farook M, et al. Risk factors for contact lens-related microbial keratitis in Singapore. Eye. 2016;30(3):447–455. https://doi.org/10.1038/eye.2015.250
- Yee A, Walsh K, Schulze M, et al. The impact of patient behaviour and care system compliance on reusable soft contact lens complications. Cont Lens Anterior Eye. 2021;44(5):101432. https://doi.org/10.1016/j.clae.2021.02.018
- Akerman D. Our greatest opportunity. Cont Lens Anterior Eye. 2018;41(4):319–320. https://doi.org/10.1016/j.clae.2018.05.007
- Booysen D. Contact: Clinical contact lens practice. 1st ed. Chennai: Notion Press; 2018, p. 181–216.
- Health Professions Council of South Africa (HPCSA). Clinical guidelines: Fitting of contact lenses [homepage on the Internet]. 2019 [cited 2020 Nov 19]. Available from: https://www.hpcsa.co.za/Uploads/ODO_2019/Clinical%20guidelines%20on%20the%20Fitting%20of%20Contact%20Lenses.pdf
- Dumbleton KA, Woods CA, Jones LW, et al. The relationship between compliance with lens replacement and contact lens-related problems in silicone hydrogel wearers. Cont Lens Anterior Eye. 2011;34(5):216–222. https://doi.org/10.1016/j.clae.2011.03.001
- Morgan PB, Efron N, Toshida H, et al. An international analysis of contact lens compliance. Cont Lens Anterior Eye. 2011;34(5):223–228. https://doi.org/10.1016/j.clae.2011.08.001
- Woolson R, Bean J, Rojas P. Sample size for case-control studies using Cochran’s Statistic. Biometrics. 1986;42(4):927–932. https://doi.org/10.2307/2530706
- Bartlett JE, Kotrlik JW, Higgins C. Organizational research: Determining appropriate sample size in survey research. Inf Technol Learn Perform J. 2001;19(1):43–50. https://doi.org/10.5032/jae.2002.03001
- Hazelrigg L. Inference. In: Hardy M, Bryman A, editors. The Handbook of data analysis. London: Sage; 2009, p. 65. https://doi.org/10.4135/9781848608184
- Cant M, Gerber-Nel C, Nel D, et al. Marketing research. 2nd ed. Pretoria: Van Schaik Publishers; 2008.
- Mishra P, Pandey CM, Singh U, et al. Descriptive statistics and normality tests for statistical data. Ann Card Anaesthesia. 2019;22(1):67–72. https://doi.org/10.4103/aca.ACA_157_18
- Kim HY. Statistical notes for clinical researchers: Assessing normal distribution (2) using skewness and kurtosis. Restor Dent Endod. 2013;38(1):52–54. https://doi.org/10.5395/rde.2013.38.1.52
- McHugh ML. The chi-square test of independence. Biochem Med. 2013;23(2):143–149. https://doi.org/10.11613/bm.2013.018
- Kim TK. Understanding one-way ANOVA using conceptual figures. Korean J Anesthesiol. 2017;70(1):22–26. https://doi.org/10.4097/kjae.2017.70.1.22
- Statistics South Africa (Stats SA). 2020 Mid-year population estimates [homepage on the Internet]. 2020 [cited 2021 Jan 06]. Available from: http://www.statssa.gov.za/publications/P0302/P03022020.pdf
- Makrynioti D, Andrikopoulos A, Grivokostopoulou F, et al. Contact lens use and compliance in Greece. Cont Lens Anterior Eye. 2019;42(6):e11. https://doi.org/10.1016/j.clae.2019.10.038
- Cope JR, Collier SA, Rao MM, et al. Contact lens wearer demographics and risk behaviors for contact lens-related eye infections – United States. MMWR Morb Mortal Wkly Rep. 2015;64(32):865–870. https://doi.org/10.15585/mmwr.mm6432a2
- Gwata S. Factors associated with soft contact lens replacement non-compliance of wearers in Windhoek [homepage on the Internet] [Masters dissertation]. Windhoek: The University of Namibia. 2017 [cited 2020 Nov 02]. Available from: http://hdl.handle.net/11070/2062
- Khoza N, Moodley T, Sokhulu S, et al. Knowledge, attitudes and practices of contact lens use in a South African adolescent population. Afr Health Sci. 2020;20(2):768–774. https://doi.org/10.4314%2Fahs.v20i2.29
- Bakkar MM, Alzghoul EA. Assessment of compliance with contact lens wear and care among university-based population in Jordan. Cont Lens Anterior Eye. 2020;43(4):395–401. https://doi.org/10.1016/j.clae.2020.02.020
- Rueff EM, Wolfe J, Bailey MD. A study of contact lens compliance in a non-clinical setting. Cont Lens Anterior Eye. 2019;42(5):557–561. https://doi.org/10.1016/j.clae.2019.03.001
- Wu Y, Carnt N, Stapleton F. Contact lens user profile, attitudes and level of compliance to lens care. Cont Lens Anterior Eye. 2010;33(4):183–188. https://doi.org/10.1016/j.clae.2010.02.002
|