Abstract
Background: Progressive additive lenses (PALs) are an increasingly prescribed form of optical compensation to correct refractive error with presbyopia but sometimes with noticeable restrictions that can reduce visual satisfaction.
Aim: The current study evaluated vision satisfaction rate and any associated problems among Saudi PAL wearers.
Setting: The study was conducted in Al-Qassim and Al-Riyadh regions, Saudi Arabia.
Methods: A cross-sectional design was used with a Likert-scale questionnaire survey (LQS) in this study. Data were analysed using Statistical Package for Social Sciences (SPSS) software version 21, Graphpad Prism, and MS Excel programmes, and p < 0.05 was considered statistically significant.
Results: One hundred and thirty-eight Saudi PALs wearers (87 men [63%] and 51 women [37%]) aged over 40 years participated in the study. Participants completed an online questionnaire concerning their levels of visual satisfaction and reported any complaints while using PALs. The overall results indicated high levels of satisfaction with comfortable vision in all tasks (median = 4 on LQS) with 55% overall vision satisfaction (p = 0.001). A strong association was found between the overall vision satisfaction and seeing when driving, and, also, with reading (p < 0.001). The length of time since starting the use of PALs was found to be significantly (p = 0.001) associated with overall satisfaction and associated complaints, while gender and age had no impact on overall vision satisfaction.
Conclusion: Saudi PAL wearers possess a good level of visual satisfaction while experiencing some difficulties and complaints when using their PALs. Gender and age were not factors that impacted overall visual satisfaction and complaints; however, time since starting to wear PALs was a factor.
Keywords: progressive addition lenses; presbyopia; visual comfort; visual satisfaction.
Introduction
Progressive lenses are also called progressive addition lenses (PALs), or progressive power lenses (PPLs), varifocals or multifocals and they are used to correct refractive error with presbyopia, in myopia control and with other accommodation disorders.1 Presbyopia is an age-related decrease in ocular accommodation that reduces the ability of the eyes to focus on close objects.2,3,4,5,6 Previous studies have compared different types of presbyopic corrections and have suggested that PALs are the most acceptable solution.7,8,9,10 A PAL is designed to provide continuous vision at all required viewing distances (distance, intermediate and near).1,5 Progressive lenses ensure the optimal dioptric power for every distance that the presbyopic spectacle wearer requires, for smooth and uninterrupted vision without any visible lines of demarcation.11 However, in eccentric viewing PAL wearers experience blurred and distorted vision (‘swimming effects’) through the peripheral parts of the lens that may increase the risk of falling. Moreover, wearers of PALs suffer dizziness and vertigo as well as problems in reading at both near and intermediate distances when changing gaze horizontally because of restricted optical zones.12,13 This will lead to increments in compensatory head movements to get clear vision. These effects can be appreciably reduced by coordination of eye and head movements and proper centration of lenses in the spectacle frame so that the visual axes of the wearer coincide with the optical centres of the PALs.14,15 Therefore, individual eye movements and optical lens characteristics are key factors for the successful wearing of progressive lenses that have importance in adaptation and satisfaction to PALs.14,15,16 Today’s PAL designs are personalised to specific prescriptions taking into account the specific vision requirements and generally provide better visual performance.17 Currently, a wide range of advanced PAL designs (using new technologies of free form, wave aberrations, etc) provide natural vision and are cosmetically acceptable.18 Furthermore, modern progressive lenses represent a compromise design that achieves better overall utility. Computer progressive lenses are ideal for people who need clear vision at intermediate and near distances.18,19,20 Special purpose PALs, for example, occupational progressives, short corridor progressive lenses and near variable progressive lenses that contain distance corrected powers, are used for office situations and computer viewing distances and advances in optical lens design have led to free-form PALs that offer a larger horizontal extent of clear vision at reading distances as well as variable corridor size.21 Flexible-design PALs permit effective placement of viewing zones according to the wearer visual needs, thus providing customised design and increasing wearer satisfaction, thus reducing or preventing complaints.16 High rate of satisfaction and comfortability were reported by PALs wearers because of the high quality of vision, the elimination of imaginary lines and image jumping.22,23 Spectacle intolerance is a common aspect in optometric practice, particularly when dealing with PALs as wearers’ expectations are high.15 Errors in dispensing or in measuring refractive errors, and adaptation difficulties, are generally the most common causes of patient dissatisfaction.24,25 A communication breakdown between the optometrist and wearer is a major cause of PALs dissatisfaction in optometric practice and in PALs acceptance by the patient. Progressive additive lenses dispensing has a direct impact on the functional use of the spectacles. A period of adaptation may be needed in new spectacle wearers, before other possible causes for the non-tolerance, for example, an error in refraction, ill-fitting and wearer education about the limitations of the lenses can be ruled out.26 Using a checklist and listening to what the patient tells you at all levels of dispensing is important to overcome PALs intolerance and enhance satisfaction.27 The role of practitioners is to ensure an optimal vision correction that offers satisfactory optical performance, wearing comfort, functionality and is cosmetically pleasing.28 The analysis of a spectacle prescription is usually the starting point of the dispensing process. Information and interpretation of a prescription statement into a usable, finished pair of spectacles that fulfils both the requirements and expectations of the user is often considered one of the most important aspects of the dispensing of a pair of spectacles.26 Understanding the purposes for which the spectacles will be used and the environment in which the patient uses them will assist practitioners to provide the ideal spectacles for a patient. The prescription analysis includes whether the prescription is satisfactory or not and discussing the prescription with the patient in relation to their visual demands.29 Integration between practitioners (optometrists and opticians) as well as users forms an essential part of the satisfying and successful wearing of PALs.30,31 Optometrists have an important role in the proper selection and fitting of the spectacle frame and lenses, such as prescription interpretation, individual visual needs, and fitting measurements and verification, and especially with PALs.32,33 Appropriate selection and glazing are specifically important with PALs, which present many variables that can lead to patient dissatisfaction, hence influencing the overall quality of vision.34,35,36,37 The ability to specify progressive corridor length requires the practitioner to possess an in-depth understanding of the interplay between the natural reading-level preferences of eyes, lens fitting parameters, individual prescription values and the design goals of the lens itself.11,38 Checking and verification for finished spectacle PALs is an important routine that ensures quality control and enhances patient satisfaction and comfort. The finished PALs spectacles are checked on the user for fitting, function and comfort, and any adjustments are made before they are handed out to the patient. A practitioner should check whether the patient achieved the optimal visual acuity with the compensating lenses and provide advice on the use of spectacles and any aftercare.28,31 A practitioner should clearly explain to the patient that an adaptation period is often required, especially for new PAL wearers, which varies from a few hours to days but not usually more than two weeks. During this period, wearers may suffer headaches and vertigo as well as mild disorientation when walking around. It is recommended that when these complaints arise, the PALs are removed for a short period and worn after complaints have lessened. To enhance adaptation to use PALs, the wearer is recommended at the first time it is better to turn their head to look at objects instead of moving the eyes from side to side and moving the eyes downwards instead of tilting the head while reading.39,40,41 To our knowledge, there is no published study conducted in Saudi Arabia concerning visual satisfaction of PALs wearers. Hence, this study aimed to evaluate the vision satisfaction rate and any associated problems among Saudi progressive lenses wearers.
Materials and methods
A cross-sectional analytical study design was used to collect the data to assess the rate of satisfaction with visual performance and PALs as built on respondents’ daily activities and any associated symptoms. Data were collected between 15 October 2021 and 15 November 2021. A total of 138 participants aged 40 years and above were selected to participate in the study. The target population was the group of individuals wearing PALs as a presbyopic refractive correction in Al-Qassim and Al-Riyadh regions, Saudi Arabia, with near additions from 1.00 dioptre (D) to 3.00 D. Those wearing PALs for myopia control or ocular accommodation disorders were excluded from this study. The study was conducted via various optical centres and the sample size was estimated by using the following formula49:
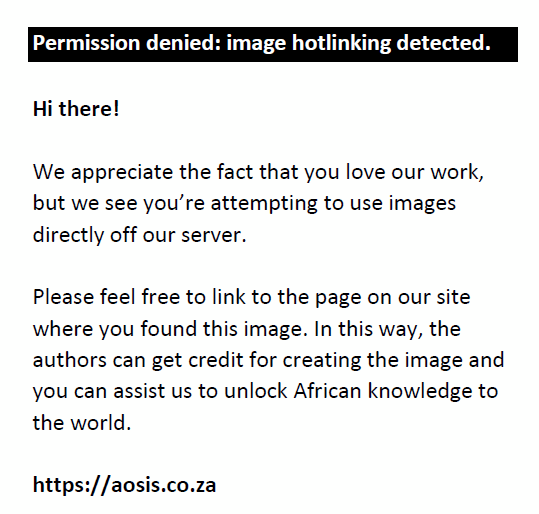
where Z = 1.96 at the 95% confidence level, P is the prevalence or proportion of the PAL wearers and is assumed to be 0.25 (decimal notation) or 25%,8 and E = the maximum acceptable sampling error (here 7% or 0.07 in decimal notation. Thus,
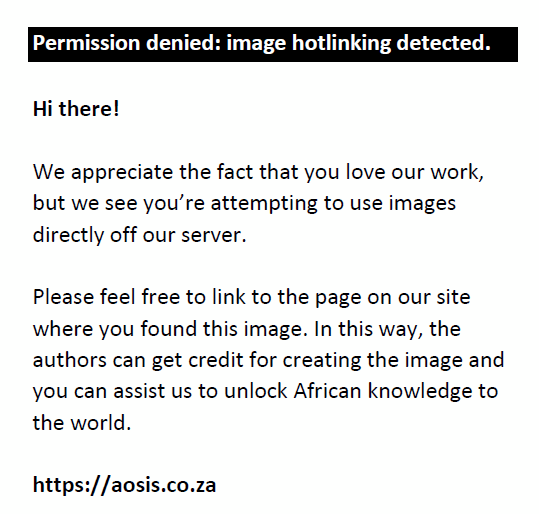
PALs wearers. A 10% non-participation rate (or 15) was assumed; so the final study sample size was calculated to be 162 PALs wearers. Verbal permission was obtained from the Optical Centre managers and participants for the collection of data. The questionnaires were distributed to the PALs wearers after they were provided with a brief explanation of the general concepts and aims of the questionnaire. Participants had the right to withdraw from the study at any stage. The respondents completed the online questionnaires as accessed through Google Forms. The questionnaire had three parts: demographic details (age, gender and how long he or she has been using PALs), feedback from respondents, as well as complaints reported by the PALs users. The participants also rated their overall satisfaction by means of a five-point Likert rating scale (from 5 = very satisfied to 1 = very dissatisfied). The questions concerned visual performances at near, intermediate and far distance, with the total satisfaction of PALs answered using this scale. Complaints that arose while wearing the PALs were similarly recorded in the questionnaire. The questionnaire was reviewed by experts in optometry and statistics, and after all their comments and observations had been considered, a pilot survey was conducted (with five respondents) to check the reliability and consistency of the questionnaire (Cronbach’s alpha = 0.71). The questionnaire was then distributed online to the respondents by means of Google Forms.
Data analysis
Data were analysed using Statistical Package for Social Sciences (SPSS) software version 21, Graphpad Prism, and Microsoft Excel. The information was evaluated for data entry mistakes and any lost values before conducting the analysis. The descriptive statistics used included frequencies, proportions (prevalence), as well as simple bar charts and curves, and an inferential analysis test of independence (association) was conducted using the Chi-square test with a 0.05 level of significance.
Ethical considerations
Ethical approval to conduct the study was obtained from the Committee of Health Research Ethics, Deanship of Scientific Research, Qassim University (clearance no. 21-02-11).
Results
A total of 138 participants with a response rate of 85.2% were enrolled in this study. The age profile of the participants was as follows: 67.0% (n = 92) under 50 years of age and 33.0% (n = 46) were more than 50 years of age. The gender profile of the participants was as follows: 63.0% (n = 87) men and 37.0% (n = 51) women. The length of time since starting use of PALs was found as six months to one year: 39.8% (n = 55), 1–2 years: 49.3% (n = 68) while > 2 years 10.9% (n = 15). The proportion of PALs wearers who are very satisfied and satisfied was 50.0%, while another 28.4% of the wearers were fairly satisfied with their progressive lenses in daily vision activities and tasks such as driving, looking at advertisement boards, shopping at markets (seeing grocery shelves), computer vision, reading and seeing their mobile phones (see Table 1 and Figure 1). As shown in Table 2, most of the respondents were comfortable and satisfied with their progressive lenses (overall median = 4; χ2 = 57.3, p = 0.001). As shown in Table 3, the proportion of PALs wearers who reported some difficulties or complaints (high and highest), such as headache, eye strain, blurring vision and vertigo, was approximately 30% (41 respondents out of 138), while most of the PALs wearers (n = 97; 70%) (moderate, least and less) reported suffering from slight difficulties or complaints (overall median = 3; χ2 = 42.29, p = 0.001; see Figure 2). Pearson’s chi-squared test showed an insignificant association between gender and overall visual satisfaction (χ2 = 24.6, p = 0.264), as well as between gender and overall symptoms (χ2 = 17.409, p = 0.235). Also, an insignificant association was found between age and overall visual satisfaction (χ2 = 17.415, p = 0.680), as well as between age and overall symptoms (χ2 = 7.543, p = 0.912). However, a highly statistically significant association was found between length of time since starting the use of PALs and overall satisfaction (χ2 = 75.088, p = 0.001), as well as between time length and overall complaints (χ2 = 59.477, p = 0.001). Analysis of the results showed that overall satisfaction was positively influenced by the satisfaction of reading with PALs, followed by using PALs while shopping (seeing grocery shelves), driving, viewing the computer, seeing mobile phones and, lastly, in viewing advertisement boards (Spearman’s correlation: ρ = 0.77, 0.76, 0.76, 0.75, 0.74 and 0.68, respectively; p = 0.001). Suffering eye strain when wearing PALs was the most obvious complaint that inversely influenced the overall level of satisfaction, which was followed by a blurring of vision, suffering headache and then suffering vertigo (Spearman’s correlation ρ = −0.46, −0.45, −0.36 and −0.33, respectively; p = 0.001) (Table 4). Spearman’s correlations test (ρ) showed a significant statistical association between quality of vision at distance viewing for driving and seeing advertisement signboards, intermediate for seeing grocery shelves and computer monitor, near for seeing on mobile phone and reading and overall visual satisfaction level (0.90; 0.91; 0.91, p = 0.000), respectively.
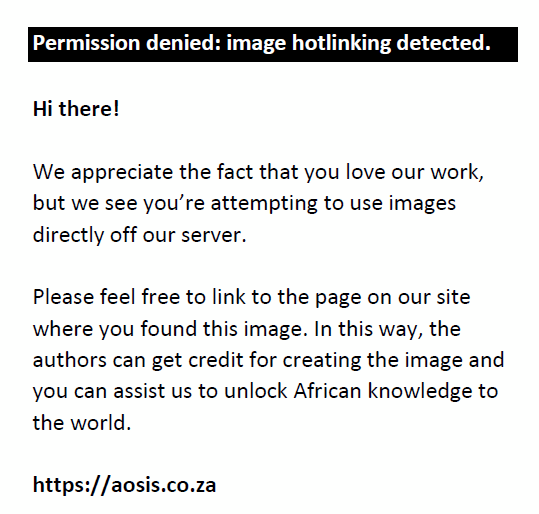 |
FIGURE 1: Vision satisfaction rates in percentages (from very dissatisfied to very satisfied). |
|
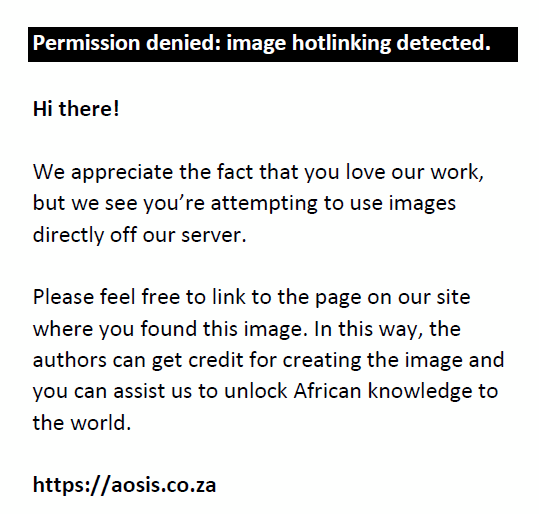 |
FIGURE 2: Respondents complaints reported associated with progressive addition lenses. |
|
| TABLE 1: Vision satisfaction rates with progressive addition lenses. |
| TABLE 2: Vision satisfaction analysis for respondents (n = 136 progressive addition lenses wearers). |
| TABLE 3: Respondent complaints associated with progressive addition lenses. |
| TABLE 4: Analysis of respondents’ reported symptoms. |
Discussion
This study investigated visual satisfaction and any associated complaints among Saudi PAL wearers. The lens designs and types provide a good solution to correct presbyopia.13,14 Practitioners need to ensure that spectacle wearers are accurately refracted and that the face and the selected frame are optimally measured and appropriate for PALs. Progressive additive lenses should be well fitted according to the manufacturer’s recommendations. Hence, the patient should be educated with an appropriate understanding and knowledge of how to use the spectacles and about possible limitations of the lenses.24 The understanding and the knowledge about the PALs lenses should disseminate between the prescribers, manufacturers, opticians and the patients themselves to achieve the best possible results for such relatively expensive lenses. Many studies have reported inappropriate fitting of the PALs, which can reduce visual satisfaction as well as increase non-tolerance.25,26
Findings of the current study revealed that the quality of vision was positively correlated with the PAL wearer’s overall levels of vision satisfaction. However, different visual tasks had unequal effects on overall satisfaction, while complaints were found to be negatively correlated with the PAL wearer vision overall satisfaction level. Furthermore, complaints had different effects on overall satisfaction. Similar results were reported by Najmee et al.34 who found that the quality of vision was positively correlated with the level of total satisfaction for PAL and inversely correlated with the reported complaints. However, blurry vision was the most prominent complaint that reduced the level of total satisfaction. In contrast, in our study, suffering eye strain when wearing PALs was the most obvious complaint that inversely influenced the overall level of satisfaction. Furthermore, the best vision quality found was when seeing grocery shelves at intermediate viewing, and the lowest quality of vision reported was by viewing at a distance while driving. In our study, the best vision quality was found when reading with PALs, followed by using PALs while shopping (seeing grocery shelves), driving, viewing the computer, seeing mobile phones and, lastly, viewing advertisement boards. The best vision quality and high level of satisfaction during near tasks indicated the appropriate PAL design preferred by wearers and adaptation to the lenses. These findings are inconsistent with the findings of Chu35 because greater head movements are required by a PALs wearer when reading a near task, which reduced the PALs wearers’ adaptation and satisfaction level. Distant quality of vision, to some extent, was found to have the lowest level of visual satisfaction, such as when driving or viewing advertisements on boards where PALs wearers are impaired by peripheral distorted field of view. Similar justifications are found in another study conducted by Ellison.36 Thus, measuring the variances at different viewing distances is of extreme importance and ultimately affects the visual task performance, as indicated by Sheedy et al.28 The findings of the current study revealed that the quality of vision at intermediate viewing with total satisfaction gave the highest correlation when compared to distant and near viewing tasks. These findings support Gispets et al.’s37 and Selenow et al.’s11 suggestions that the stimulus should be of sufficient and precise magnitude to be sensed within the clear field of view at the intermediate corridor. Our findings also revealed a high level of satisfaction with a significant positive linear correlation for near viewing tasks like reading and seeing on a mobile phone. These findings support the importance of the use of the clearest portion of the lens (the centre of the near zone) in reading, as indicated by Lynn.38 Another study found that the best quality vision was for distant viewing tasks and the worst for close reading tasks,39 which contradicts our findings. These differences might be because of differences in sample characteristics, such as age or visual needs (priorities), or might be attributed to the PAL designs. The study findings showed that the quality of vision at different viewing distances while wearing PALs had a different contribution to the overall visual satisfaction level. Thus, different viewing distances or different tasks should be looked at carefully to achieve the best quality of vision as well as a high level of visual satisfaction. In the current study, most PAL wearers (50% of the respondents) were found to be satisfied or very satisfied, which is much less than that found by Bonnin et al.40 where respondents obtained a higher rate of vision satisfaction with PALs (84%, satisfied and very satisfied). The difference might be attributed to variation in population characteristics studied or in the methodologies, differences in PAL types or designs, or possibly the length of time since starting to use the PALs. Another study by Odjimogho et al.,41 who surveyed 106 PALs wearers, reported that 69.8% of patients had a high rate of comfortability with their PALs, which is slightly greater than what we obtained in the present study. The study findings revealed that the length of time the individuals have been wearing PALs plays an important role in adaptation (χ2 = 75.088, p = 0.001) as the improvement in satisfaction is enhanced by an understanding of how to compensate for peripheral blurry vision because of astigmatism and magnification of the progressive addition design nature.42,43,44,45,46 Generally, the results show a good visual satisfaction level with slight to moderate difficulties and complaints while wearing these lenses which have an impact on overall vision satisfaction, hence reflecting the value of correcting presbyopia by spectacles, especially PALs. These findings are in line with that of Goertz et al.47 and Fafiolu et al.48 who highlighted the importance of presbyopic correction and its appreciable effect on life quality. One of the drawbacks of this study was that most of the participants were between the ages of 40 and 50 years, while the reasons for using PALs were not included in the survey. Also, the powers of the additions and whether PALs were first worn or not were not included. Further studies need to be carried out among PALs wearers, dispensing opticians and optometrists to determine the gaps in knowledge, understanding and skills in PAL practice needed for optimal improvement in vision satisfaction.
Conclusion
In this study, approximately half of the respondents were satisfied or very satisfied with their PALs. However, about 30% of the participants wearing PALs reported noticeable symptoms and difficulties. Satisfaction and symptoms experienced with the use of PALs had no association with the age or gender of the wearers. However, a strong association was found between vision satisfaction and associated symptoms and the amount of time PALs wearers had been wearing the lenses.
Acknowledgements
The author would like to thank all optical centres and PALs wearers who participated in this study.
Competing interests
The authors declare that they have no financial or personal relationships that may have inappropriately influenced them in writing this article.
Authors’ contributions
I declare that I am the sole author of this research article.
Funding information
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Data availability
Data supporting the findings of this study are available from the corresponding author, A.M.E., on request.
Disclaimer
The views and opinions expressed in this article are those of the author(s) and do not necessarily reflect the official policy or position of any affiliated agency of the authors.
References
- Pope DR. Progressive addition lenses: History, design, wearer satisfaction and trends. Optica, 2000, paper NW9. https://doi.org/10.1364/VSIA.2000.NW9
- Wubben TJ, Guerrero CM, Salum M, Wolfe GS, Giovannelli GP, Ramsey DJ. Presbyopia: A pilot investigation of the barriers and benefits of near visual acuity correction among a rural Filipino population. BMC Ophthalmol. 2014;14(1):1–7. https://doi.org/10.1186/1471-2415-14-9
- Frick KD, Joy SM, Wilson DA, Naidoo KS, Holden BA. The global burden of potential productivity loss from uncorrected presbyopia. Ophthalmology. 2015;22(8):1706–1710. https://doi.org/10.1016/j.ophtha.2015.04.014
- Wolffsohn JS, Davies LN. Presbyopia: Effectiveness of correction strategies. Prog Retin Eye Res. 2019;68:124–143. https://doi.org/10.1016/j.preteyeres.2018.09.004
- Charman WN. Developments in the correction of presbyopia I: Spectacle and contact lenses. Ophthalmic Physiol Opt. 2014;34(1):8–29. https://doi.org/10.1111/opo.12091
- Vujko Muždalo N, Mihelčić M. Individually designed PALs vs. power optimized PALs adaptation comparison. Coll Antropol [serial online]. 2015 [cited 2021 Sept 12];39(1):55–61. Available from: https://hrcak.srce.hr/file/217228
- Moussa K, Jehangir N, Mannis T, Wong WL, Moshirfar M. Corneal refractive procedures for the treatment of presbyopia. Open Ophthalmol J. 2017;11:59–75. https://doi.org/10.2174/1874364101711010059
- Fricke TR, Tahhan N, Resnikoff S, et al. Global prevalence of presbyopia and vision impairment from uncorrected presbyopia: Systematic review, meta-analysis, and modelling. Ophthalmology. 2018;125(10):1492–1499. https://doi.org/10.1016/j.ophtha.2018.04.013
- Sivardeen A, McAlinden C, Wolffsohn JS. Presbyopic correction use and its impact on quality of vision symptoms. J Optom. 2020;13(1):29–34. https://doi.org/10.1016/j.ophtha.2018.04.013
- Meister D. Fundamentals of progressive lens design. VisionCare Product News. 2006;6(9):5–9. https://doi.org/10.1111/j.1444-0938.2007.00245.x
- Selenow A, Bauer EA, Ali SR, Spencer LW, Ciuffreda KJ. Assessing visual performance with progressive addition lenses. Optom Vis Sci. 2002;79(8):502–505. https://doi.org/10.1097/00006324-200208000-00012
- Suemaru J, Hasebe S, Ohtsuki H. Visual symptoms and compliance with spectacle wear in myopic children: Double-masked comparison between progressive addition lenses and single vision lenses. Acta Med Okayama. 2008;62(2):109–117. http://doi.org/10.18926/AMO/30955
- Garcia-Espinilla O, Gallegos-Cocho I, Sanchez I, Cañadas P, Martin R. Comparison of physiognomy and frame angle parameters using different devices to prescribe progressive addition lenses. Clin Exp Optom. 2022;105(4):420–427. https://doi.org/10.1080/08164622.2021.1914511
- Bist J, Kaphle D, Marasini S, Kandel H. Spectacle non-tolerance in clinical practice-a systematic review with meta-analysis. Ophthalmic Physiol Opt. 2021;41(3):610–622. https://doi.org/10.1111/opo.12796
- Savio G, Concheri G, Meneghello R. Parametric modeling of free-form surfaces for progressive addition lens. Proc IMProVe [serial online]. 2011 [cited 2021 Oct 12];167–174. Available from: https://pdfs.semanticscholar.org/3f6b/7f35e63ab858ecb3896be670eaddfbf57eae.pdf
- Han SC, Graham AD, Lin MC. Clinical assessment of a customized free-form progressive add lens spectacle. Optom Vis Sci. 2011 [cited 2021 Sept 20];88(2):234–243. https://doi.org/10.1097/OPX.0b013e31820846ac
- Jalie M. Progressive lenses Part 1: How progressive power is obtained. Contin Educ Train [serial online]. 2005 [cited 2021 Oct 10];2:31–40. Available from: https://www.yumpu.com/en/document/view/25242417/progressive-lenses-part-1-how-progressive-power-is-obtained
- Forkel J, Reiniger JL, Muschielok A, Welk A, Seidemann A, Baumbach P. Personalized progressive addition lenses: Correlation between performance and design. Optom Vis Sci. 2017;94(2):208–218. https://doi.org/10.1097/OPX.0000000000001016
- Meister DJ, Fisher SW. Progress in the spectacle correction of presbyopia. Part 1: Design and development of progressive lenses. Clin Exp Optom. 2008;91(3):240–250. https://doi.org/10.1111/j.1444-0938.2007.00245.x
- Meister DJ, Fisher SW. Progress in the spectacle correction of presbyopia. Part 2: Modern progressive lens technologies. Clin Exp Optom. 2008;91(3):251–264. https://doi.org/10.1111/j.1444-0938.2008.00246.x
- Tang Y, Quanying Wu, Chen X, Zhang H. A personalized design for progressive addition lenses. Opt Express. 2017;25(23):28100–28111. https://doi.org/10.1364/OE.25.028100
- Farrell J. Dispensing causes of non-tolerance. Optician. 2005;229:22–26.
- Alvarez TL, Kim EH, Granger-Donetti B. Adaptation to progressive additive lenses: Potential factors to consider. Sci Rep. 2017;7(1):1–4. https://doi.org/10.1038/s41598-017-02851-5
- Hrynchak P. Prescribing spectacles: Reasons for failure of spectacle lens acceptance. Ophthalmic Physiol Opt. 2006;26(1):111–115. https://doi.org/10.1111/j.1475-1313.2005.00351.x
- Keirl A. Essential course in dispensing: Part 1 – Interpreting the prescription. Optician [serial online]. 2013;245:12. Available from: https://www.opticianonline.net/cpd-archive/14
- U.S. Food and Drug Administration. Multifocal visual performance study – Seamless transition with precision profile MF lenses. Food Drug Law Weekly. 2018;464:1–12.
- Bell GR. Verifying and evaluating progressive addition lenses in clinical practice. Optometry. 2001;72(4):239–246. https://doi.org/10.1111/j.1475-1313.2005.00351.x
- Sheedy J, Hardy RF, Hayes JR. Progressive addition lenses-measurements and ratings. Optometry. 2006;77(1):23–39. https://doi.org/10.1016/j.optm.2005.10.019
- Elliott DB, Howell-Duffy C. ‘Non-tolerances’ and the science of prescribing spectacles. Optom Pract [serial online]. 2015 [cited 2021 Oct 12];16(4):131–144. Available from: https://docplayer.net/20781685-Non-tolerances-and-the-science-of-prescribing-spectacles.html
- Mohan K, Sharma A. How often are spectacle lenses not dispensed as prescribed? Indian J Ophthalmol. 2012;60(6):553–555. https://doi.org/10.4103/0301-4738.103796
- Freeman CE, Evans BJ. Investigation of the causes of non-tolerance to optometric prescriptions for spectacles. Ophthalmic Physiol Opt. 2010;30(1):1–11. https://doi.org/10.1111/j.1475-1313.2009.00682.x
- Sheedy JE. Progressive addition lenses-matching the specific lens to patient needs. Optometry. 2004;75(2):83–102. https://doi.org/10.1016/S1529-1839(04)70021-4
- Brown P. Professional pearls for fitting PALs: Here are some tips you need to know to properly fit your patients’ progressive lenses. Rev Optom [serial online]. 2007 [cited 2021 Feb 28];144(1):31–35. Available from: https://www.reviewofoptometry.com/article/professional-pearls-for-fitting-pals
- Najmee NA, Buari NH, Mujari R, Rahman MI. Satisfaction level of progressive additional lens (PAL) wearers. Environ Behav Proc J. 2017;2:373–382. https://doi.org/10.21834/e-bpj.v2i6.999
- Chu BS. The impact of presbyopic spectacles and contact lenses on driving performance [doctoral dissertation] [cited 2021 Nov 12]. Queensland University of Technology. Available from: https://eprints.qut.edu.au/31885/1/Byoung_Chu_Thesis.pdf
- Ellison A. Prismatic displacement effect of progressive multifocal glasses on fall risk in elderly people [doctoral dissertation] [cited 2021 Nov 15]. University of Otago. Available from: http://hdl.handle.net/10523/2475
- Gispets J, Arjona M, Pujol J, Vilaseca M, Cardona G. Task oriented visual satisfaction and wearing success with two different simultaneous vision multifocal soft contact lenses. J Optom. 2011;4(3):76–84. https://doi.org/10.1016/S1888-4296(11)70046-2
- Lynn J. Progressive addition spectacle lenses: Design preferences and head movements while reading [PhD thesis] [cited 2021 Oct 20]. The Ohio State University; 1998. Available from: https://ui.adsabs.harvard.edu/abs/1998PhDT…….118P/abstract
- Solaz JS, Porcar-Seder R, Mateo B, et al. Influence of vision distance and lens design in presbyopic user preferences. Int J Ind Ergon. 2008;38(1):1–8. https://doi.org/10.1016/j.ergon.2007.07.006
- Bonnin T, Torrilhon V. Study on the satisfaction of people who wear progressive lenses, conducted in optical shops [homepage on the Internet]; 2018 [cited 2021 July 12]; p. 1–6. Available from: http://pointsdevue.com
- Odjimogho ES, Odjimogho SE. Survey on problems associated with the use of progressive addition lenses (pal). J Niger Optom Assoc. 2004 [cited 2021 Sept 17];11. https://doi.org/10.4314/jnoa.v11i1.64440
- Elliott DB, Hotchkiss J, Scally AJ, Foster R, Buckley JG. Intermediate addition multifocals provide safe stair ambulation with adequate ‘short-term’ reading. Ophthalmic Physiol Opt. 2016;36(1):60–68. https://doi.org/10.1111/opo.12236
- Chamorro E, Cleva JM, Concepción P, Subero MS, Alonso J. Lens design techniques to improve satisfaction in free-form progressive addition lens users. JOJ Ophthalmol. 2018;6(3):555688. https://doi.org/10.19080/JOJO.2018.06.555688
- Parveen S, Mobin R. Adaptation period of different refractive prescriptions in pre-presbyopic adults. Ophthalmol Pakistan [serial online]. 2017 [cited 2021 Aug 25];7(02):24–30. https://www.ophthalmologypakistan.com/op/index.php/OP/article/viewFile/172/134
- Alvarez TL, Han S, Kania C, et al. Adaptation to progressive lenses by presbyopes. 4th International IEEE/EMBS Conference on Neural Engineering, Antalya, Turkey; 2009 Apr 29. IEEE, 2009; p. 143–146.
- Jarosz J, Molliex N, Chenon G, Berge B. Adaptive eyeglasses for presbyopia correction: An original variable-focus technology. Opt Express. 2019; 27(8):10533–10552. https://doi.org/10.1364/OE.27.010533
- Goertz AD, Stewart WC, Burns WR, Stewart JA, Nelson LA. Review of the impact of presbyopia on quality of life in the developing and developed world. Acta Ophthalmol. 2014;92(6):497–500. https://doi.org/10.1111/aos.12308
- Fafiolu VO, Ajibod HA, Onabolu OO, Jagun KO, Bodunde OT, Otulana TO. The impact of presbyopia on the quality of life in a semi-urban community in Southwest Nigeria. Afr Vision Eye Health. 2020;79(1):a548. https://doi.org/10.4102/aveh.v79i1.548
- Charan J, Biswas T. How to calculate sample size for different study designs in medical research? Indian J Psychol Med. 2013;35(2):121–126. https://doi.org/10.4103/0253-7176.116232
|




