Abstract
Background: Global estimates suggest there are almost 19 million visually impaired children worldwide, the major cause being uncorrected refractive error (RE).
Aim: To assess the prevalence of visual impairment (VI) and RE among Sudanese school-aged children.
Setting: Eight randomly selected primary schools from 21 districts in South Darfur State of Sudan were involved.
Methods: A school-based cross-sectional study of RE and VI in primary schoolchildren from grades 1 to 8 (children aged 6–15 years) was investigated. A Refractive Error Study in Children (RESC) protocol was implemented to determine the prevalence of RE and VI in these school-aged children. Participants were enrolled through stratified multistage cluster sampling of four all-male and four all-female primary schools from South Darfur State of Sudan. Examination procedures followed the RESC protocol, which included visual acuity (VA) measurements, binocular vision assessments, retinoscopy and autorefraction under cycloplegia, as well as examination of the external eye, anterior-segment, media and fundus.
Results: A total of 1775 children were invited to participate in the study and 1678 were examined resulting in a participation rate of 94.5%. The findings indicated that the prevalence of uncorrected, presenting and best-corrected VA of 6/12 or worse was 6.4% (95% confidence interval [CI], 4.9–7.9), 4.4% (95% CI, 2.9–5.9) and 1.2% (95% CI, 0.3–2.7) respectively. RE was the cause of VI in 57% of participants, retinal disorders in 13.1%, amblyopia in 5.6%, corneal opacity in 0.9%, cataract in 3.7%, with the causes of reduced vision undetermined in 10.3% and various other causes contributed 9.3%. External and anterior-segment abnormalities were observed in 10.2% of children. This was mainly allergic conjunctivitis (5.3%) followed by bacterial and viral conjunctivitis (4.2%). The prevalence of myopia (≥|-0.50 D|) in one or both eyes was 6.8% (95% CI, 5.3–8.3), hypermetropia (≥ 2 D) was noted in 1.9% (95% CI, 0.4–3.4) and astigmatism (≥|-0.75 D|) prevailed in 2.5% (95% CI, 1.0–4.0). Prevalence of VI among school-aged children were associated with the children’s age and grade levels (p = 0.00) but was not correlated with gender (p = 0.224). Prevalence of RE among school-aged children was significantly correlated with age and grade levels (p = 0.00). No significant correlation was found between gender and prevalence of RE (p = 0.833). The prevalence of VI because of myopia was associated with increasing grade levels and also the childhood age (p = 0.023), but there was no significant difference in the prevalence of VI because of myopia between male and female children.
Conclusion: Uncorrected RE was a major cause of VI among children in the South Darfur State. There is thus a critical need for developing a comprehensive child eye care plan focusing on the reduction of uncorrected RE through collaboration between key stakeholders and government.
Introduction
Global estimates indicate that there are around 19 million visually impaired children worldwide; of these, 1.4m are blind and 17.5m have low vision with many of them living in Africa.1 In a recent classification by the World Health Organization (WHO), the major cause of worldwide vision impairment was uncorrected refractive error (RE).1 Current worldwide estimate indicates that more than 90% of people with uncorrected RE live in rural and developing nations.2 WHO defines visual impairment (VI) in children as presenting visual acuity (VA) less than 6/12 in the better eye.3 However, uncorrected visual acuity (UVA) is defined as VA less than 6/12 in one or both eyes. VI among children in poor countries is one of the priorities of many eye health programmes including the Vision 2020: the Right to Sight initiative.3 Children presenting with VI means that the impact of such impairment is perhaps much more critical because of the potentially longer duration of their lives as compared to older people; however, some studies have estimated that almost 60% of children die within 1 year of becoming blind.3,4 A population-based study on VI and RE in school-aged children that began in 1998, using the same protocol, Refractive Error Study in Children (RESC), was conducted on populations with different racial backgrounds and environments.5 This RESC protocol was developed by the WHO in collaboration with, and under financial support from the National Eye Institute, National Institutes of Health (NIH) and the United States.6 Published studies using this protocol have been conducted in different countries including South Africa,7 China,8 India,9 Brazil10 and Saudi Arabia.11 These studies have shown that the prevalence of VI among school-aged children in South Africa is 2.1%,7 in India 6.4%9 and 2.6% in Brazil. The prevalence of myopia, hypermetropia and astigmatism among African school-aged children in South Africa were 4.0%, 2.6% and 14.6%, respectively.7 Uncorrected RE drives children and adults further into poverty by limiting their opportunities to education and employment and this could seriously affect their quality of life and productivity.12 After the 1990s, two papers from Australia and India emphasised the fact that uncorrected RE was a major cause of VI in children.13 The WHO and the International Agency for Prevention of Blindness have included uncorrected RE to the prevention of blindness agenda and have developed strategies for the elimination of this simple yet avoidable cause of VI.13
Sudan is the second largest country in Africa geographically covering an area of about 1.8 million square kilometres, with an estimated population of more than 39m inhabitants.14 Sudan recently reached 20% inflation with a shrinking economy and is facing American sanctions. In terms of the Human Development Index, Sudan is ranked as a low-income country.14 Health indicators such as the under-5 mortality rate are 78 per 1000 live births and the average life expectancy at birth is predicted to be 60 years.15 The prevalence of VI and blindness among internally displaced children in Khartoum was 5.5% and 2.7%, respectively.16 According to the Vision 2020 programme in Sudan,17 the prevalence of blindness in the Northern States, excluding Darfur, has reduced from 1.5% in 2003 to 1.0% in 2010.17 South Darfur is located in the western part of Sudan and is one of the five states that comprise the region of Darfur.18 South Darfur is the most populous state with a population of approximately 4.45m people.19 The majority (62.7%) of people in this state live below the poverty line according to the Household Survey 2009.20 No studies have been conducted to estimate the prevalence of VI and RE in school-aged children in South Darfur State of Sudan. The aim of the present study was therefore to determine the prevalence of VI and RE in this population group. The study objectives were to estimate the main causes of VI and types of RE and to determine the difference in prevalence between gender, age and school-grade levels.
Methods
Study design
This was a cross-sectional, school-based study of VI and RE among children from the South Darfur State of Sudan. The research focused on primary schoolchildren in the 6- to 15-year age range. According to the Ministry of Education, the overall number of learners enrolled in primary schools in South Darfur during 2014–2015 was 338 068 school-aged children consisting of 187 270 boys and 150 798 girls, from public and private schools.21 An RESC protocol was implemented in order to determine the prevalence of VI and RE in these children. The protocol defines RE when carried out by cycloplegic auorefractometer as follows: (1) myopia at least −0.5 D in one or both eyes, (2) hypermetropia at least 2 D in one or both eyes and (3) astigmatism at 0.75 D or more cylindrical refraction.22
Inclusion criteria
Children aged 6–15 years and who are able to provide parental consent and all children attending the school on the examination days were included in the study.
Exclusion criteria
The exclusion criteria included those whose age did not correspond to the defined age group and those unable to provide parental consent.
Sample selection
The study sample was selected through stratified multistage cluster sampling. Assuming a prevalence of RE (P) = 5% and the worst acceptable prevalence (P) = 4%, according to the estimated prevalence of RE in Africa (5%), South Africa (4%)7 and Kenya (5.1%).23 The sample size was calculated using the sample size calculation for eye survey formula24:
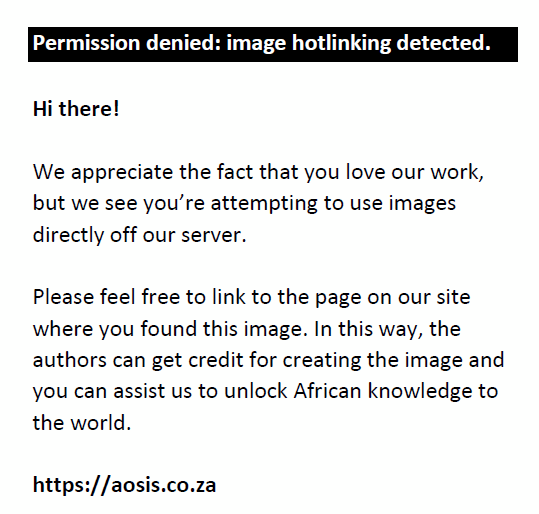
and
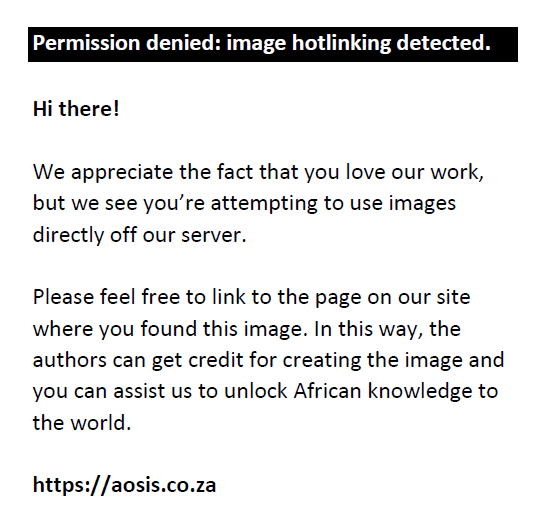
where n = minimum sample size required (approximate); N = total number of schoolchildren in the South Darfur State, in the academic year 2015 = 338 068 with Z = value of z statistic at 95% confidence level = 1.96; P = assumed prevalence of children with RE = 5%; Q = 100% – P = 95%; E = maximum acceptable random sampling error = 1.5%; W = the likely design effect = 2 was considered as we employed the cluster random sampling method. The value 3.8416 is 1.96² corresponding to Z at 95 probability of not exceeding E. In addition, the sample size was adjusted for an anticipated 10% absenteeism and non-participation rate. The final sample size was 1775 schoolchildren where eight schools (four for males and four for females) were randomly selected from the sampling frame of 21 districts of the South Darfur State. The study sample consisted of six public schools and two private schools randomly selected according to the list obtained from Ministry of Education. Within each school, the class levels represented the third stage of the sampling unit. One class from each grade (1–8) with a minimum cluster size of 28 children was randomly chosen.
Recruitment of the schoolchildren
Each school selected for the study sample was visited by the principal investigator to explain the purpose of the study to the school administration, and schoolchildren were given requests for consent and permission forms for their parents to allow them to participate in the study. Parents were asked to sign the consent letters if they agreed to allow their children to participate in the study; thereafter, such children were invited to take part in the study.
Training of the assistant researchers
Optometric research assistants with at least 3 years of experience in clinical optometry were recruited to assist with data collection. The research assistants underwent intensive training in the study protocol procedures. The principal investigator explained and demonstrated these methods in five sessions.
Pilot study
A pilot study was conducted outside the main area of study on 100 children not included in the study sample. The data collected were captured and analysed using the Statistical Package for Social Science (SPSS) Version 22. The results indicated that, some children in the vision examination reported that they had a problem in their vision but after detailed assessment of refraction, together with outer eye and inner eye examination, the results revealed that there was no abnormality in their eyes. In others, their vision examination result was normal after examination of refraction, but the outer eye and/or inner eye results demonstrated that they did in fact have eye problems. This was because of a misunderstanding of the vision examination by schoolchildren or some of them did this to get free medication and spectacles. Because the principal investigator indicated in the child’s consent form that any participants, with eye problems, would be provided free spectacles and eye drops, this could have contributed to this anomaly. Therefore, to overcome this problem in the main study, the principal investigator rechecked the VA for each child after examinations to ensure the accuracy of the measurement of VA.
Ethical and legal consideration
Ethical permission for conducting the study was obtained from the University of KwaZulu-Natal’s Biomedical Research Ethics committee (ref: BE247/14) and the National Research Ethics Review Committee in Sudan. Permission was also obtained from the South Darfur authorities in Sudan to undertake the research at their facilities. Informed consent was obtained from all participants included in the sample study to facilitate a better understanding of conditions of involvement in the study. The research was conducted in accordance with the Declaration of Helsinki.
Clinical examinations
Examination procedures employed a modified RESC protocol. Distance VA was assessed using Snellen Tumbling E-chart with E’s of standard size at a 6-meter distance. Children with VA ≤ 6/12 were tested by pinhole and if their VA improved, they underwent cycloplegic refractions. All the schoolchildren underwent a penlight and low-power hand magnifier examination to rule out any anterior-segment abnormalities in the following parts of the eye: eyelids, conjunctiva, cornea, the pupil and pupillary reflex reaction. A cover test was conducted for phorias or tropias and deviations were measured using the corneal light reflex (Hirschberg test) and the Prism Cover Test at distance and near fixation, respectively. The learners underwent motility tests to assess eye muscle function. Subjective refractions were performed by achieving best-corrected VA; while cycloplegic refractions were done for the learners where vision improved with pinhole. First one drop of ophthalmic topical anaesthetic was instilled in each eye, followed by a waiting period of 2 min to achieve ocular surface anaesthesia. Thereafter, children received two drops of 1% cyclopentolate administrated 5 min apart to each eye. If cycloplegia was not completed, then a third drop was administered as required. Cycloplegia was considered to be completed if the pupil dilated to 6 mm or greater and light reflex was absent. After cycloplegia, optometrists refracted learners, regardless of VA: using a Hand Held Auto Refractor/Keratometer (Retinomax K-plus 3). The children with VA ≤ 6/12 whose vision did not improve by pinhole test had ocular and fundus examination by direct ophthalmoscopy and any abnormal findings were recorded. Learners presenting with eye organic defects were referred for further treatment (Figure 1).
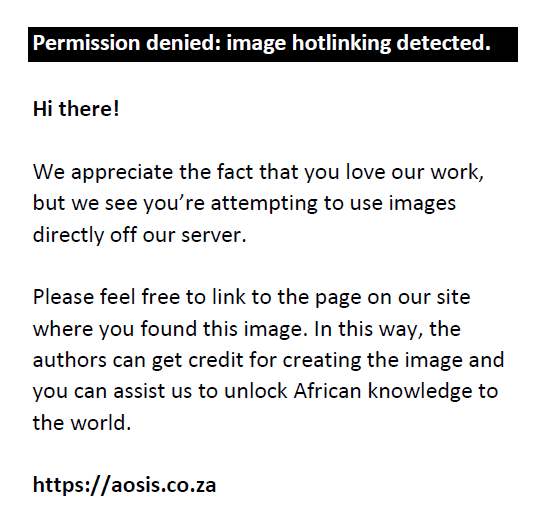 |
FIGURE 1: Chart illustrating the procedures for assessing vision and detecting vision impairment. |
|
Data analysis
Data forms were reviewed for accuracy and completeness before data capture. The data entry was performed by the principal investigator using SPSS (Version 22), the data were checked for data entry errors and/or missing values before data analysis. The data for each subject were analysed descriptively using standard deviations, modes and percentages. The relationship between measures was determined using correlation, cross-tabulations and chi-squared analysis. The analysis of variance (ANOVA) was used for statistical comparison of means. For all statistical determinations, significance levels were established at p = 0.05.
Results
Study population
Of the 1775 school-aged children selected to participate in the study, 1678 children presented at schools on the examination days resulting in a participation rate of 94.5%. The records of 12 students who were actually older than 15 years were eventually excluded from the study; thus, the results of 1666 children were analysed as discussed below.
Socio-demographic characteristics of participants
The age of the children ranged from 6 to 15 years with mean age of 10.8 ± 2.8 years (s.d.) while the median age was 11.00 years and modal age was 14 years. There were 839 female children representing 50.4% and 827 male children representing 49.6% of the sample. The mean ages and standard deviations of female and male children were 11.00 ± 2.7 years (s.d.) and 11.00 ± 2.9 years (s.d.), respectively. The age groups most represented were 14 and 12 years at 12.4% and 11.5%, respectively. The groups least represented were 6 years at 5.6%. The differences between the mean ages of male and female children was significant (ANOVA: F = 5.71, p = 0.017). Grades 1 and 2 had the highest proportion of respondents at 14.5% and 13.7%, respectively. This was followed by grades 5 and 7 at 13.20% and 12.30%, respectively, and the lowest proportion was grade 6 at 10.7%. The differences in the mean ages of the children in the classrooms were significant (ANOVA: F = 1219.092, p = 0.00).
Distribution of signs and symptoms among school-aged children
A total of 1137 (68.2%) of respondents did not complain of any ocular symptoms. In all, 180 (10.8%) complained of blurred vision, followed by 125 (7.5%) who had itching, 92 (5.5%) who had photophobia and pain, 69 (4.1%) had discharge and redness, 40 (2.4%) complained of foreign body sensation and tearing, 19 (1.1%) complained of headaches, while only 4 (0.2%) complained of difficulty seeing at night.
Visual acuity
A total of 1467 (88.1% [95% confidence interval {CI}, 86.6–89.6]) children presented with normal VA (6/6) in the right eye and 1465 (87.9% [95% CI, 86.4–89.4]) children had normal VA in the left eye with 1491 (89.5% [95% CI, 88.0–91.0]) children having normal VA in the better eye. A total of 109 (6.5% [95% CI, 5.0–8.0]), 109 (6.5% [95% CI, 5.0–8.0]), and 101 (6.1% [95% CI, 4.6–7.6]) children had uncorrected VA of (6/9) in the right, left, and better eye, respectively. About 90 children (5.4% [95% CI, 3.9–6.9]) had uncorrected VA ≤ 6/12 in the right eye and 92 (5.5% [95% CI, 4.0–7.0]) in the left eye. Uncorrected VA ≤ 6/12 in one or both eyes was found in 107 children (6.4% [95% CI, 4.9–7.9]), while 74 (4.4% [95% CI, 2.9–5.9]) children had uncorrected VA ≤ 6/12 in the better eye. With best-corrected vision, this decreased to 20 (1.2% [95% CI, 0.3–2.7]) children as shown in (Table 1).
| TABLE 1: Distribution of uncorrected visual acuity for right, left and better eye and best-corrected visual acuity by percentage and confidence interval. |
Prevalence of visual impairment
The findings of VI among 1666 school-aged children are shown in Table 2. The prevalence of VI with the uncorrected VA in the better eye ≤ 6/12 was 74 (4.4% [95% CI, 2.9–5.9]). None of these children were found to be wearing eye glasses. The prevalence of VI increased according to age. Younger ages were associated with lower prevalence: 3.0% (95% CI, 1.5–4.5) in children aged 6–7 years, 5.2% (95% CI, 3.7–6.7) in those aged 10–11 years and 6.4% (95% CI, 4.9–7.9) in those aged 12–13 years. However, there was no marked difference (p = 0.224) in the prevalence of VI between male and female children at 4.8% (95% CI, 3.3–6.3) and 4.1% (95% CI, 2.6–5.6), respectively. The prevalence of VI among school-aged children was statistically significant for the association between age and grade levels (p = 0.00).
| TABLE 2: Prevalence of visual impairment among school-aged children by age groups, gender and school grade. |
Binocular motor function
Heterotropia or heterophoria were found in 852 (51.1%) children at the 50-cm fixation distance and in 95 children (5.7%) at the 6-m fixation distance. Most of the children had exophoria at near 781 (46.9%). Tropia was observed in five (0.30%) children; three children had esotropia and two had exotropia.
Anterior-segment examination
A total of 1496 (89.8% [95% CI, 88.3–91.3]) children had no abnormalities detected, followed by 89 (5.3% [95% CI, 3.8–6.8]) children who had allergic conjunctivitis. Other eye conditions were conjunctivitis (bacterial and viral), cataract and corneal opacity at 70 (4.2% [95% CI, 2.7–5.7]), 4 (0.24% [95% CI, 1.26–1.74]) and 1 (0.06% [95% CI, 1.44–1.56]), respectively (Table 3).
| TABLE 3: Distribution of normal and external eye disease by percentage and confidence interval. |
Prevalence of refractive error
The prevalence of RE was estimated based on presenting VA (UVA of 6/9 or worse in one or both eyes). Myopia was defined as the spherical equivalent of at least |-0.5 D|, hypermetropia as 2 D or more and astigmatism as |-0.75 D| or more. The RE in one or both eyes was evaluated based on cycloplegic autorefraction. The results of the prevalence of RE in one or both eyes are presented in Table 4 by age, gender and school grades. The overall prevalence of RE among schoolchildren was 178 (11.2% [95% CI, 9.7–12.7]). Prevalence was higher among female children totalling 99 (11.8% [95% CI, 10.3–13.3]) than male children totalling (10.6% [95% CI, 9.1–12.1]), and significantly more among children aged 15 years totalling 28 (15.5% [95% CI, 14.0–17.0]), compared to 14.5%, 13.3% and 12.0% in those age 14, 13, and 12 years, respectively. The prevalence of RE showed an increasing trend from 9.1% (95% CI, 7.610.6) in grade 1 to 12.7% (95% CI, 11.214.2) in grade 8. The prevalence of RE was statistically significant for the association with both age and grade level (p = 0.00). However, the prevalence of RE was not significantly associated with gender of the schoolchildren (p = 0.833).
| TABLE 4: The prevalence of refractive error in one or both eyes by age, gender and school grade. |
Myopia, hypermetropia and astigmatism were prevalent in 114 (6.8% [95% CI, 5.3–8.3]), 31 (1.9% [95% CI, 0.4–3.4]) and 42 (2.5% [95% CI, 1.0–4.0]) children, respectively. The prevalence of myopia was more common in 15–year-old children (23; 11.1% [95% CI, 9.6–12.6]) than in young children aged 7, 8, 9 and 10 years wherein the prevalence was 2.9%, 4.1%, 6.2% and 3.7%, respectively. Myopic prevalence was not significantly different between male (6.9% [95% CI, 5.4–8.4]) and female (6.8% [95% CI, 5.3–8.3]) children. Similarly, the prevalence of hypermetropia among male and female children was not significantly different at 1.8% (95% CI, 0.3–3.3) and 1.9% (95% CI, 0.4–3.4) respectively. The prevalence of astigmatism was more common among females at 26 (3.1% [95% CI, 1.6–4.6]) than males at 16 (1.9% [95% CI, 0.4–3.4]). Moreover, the prevalence of hypermetropia was higher among 13 year olds (4.2%) followed by 15 year olds (2.8%) and lower for the ages 10, 8, and 6 years, which was 0.6%, 0.6% and 1.1%, respectively. The prevalence of myopia compared with emmetropia was statistical significant (p = 0.023) and associated with increasing grade level, whereas it was not significant (p = 0.073) with the children’s age.
The prevalence of the children who needed refractive correction in one or both eyes was 187 (11.2%) but no child presented with spectacles. The need for spectacles was the highest for both genders in the higher-grade levels.
Posterior-segment examination
Posterior-segment examination revealed that a total of 1631 (97.9% [95% CI, 96.4–99.4]) children had no abnormalities. Media and fundus abnormalities were observed in 35 (2.1%) children. Retinal disorders occurred in 17 (1.0% [95% CI, 0.5–2.5]) children. Vitreous abnormalities were present in 4 (0.2% [95% CI, 1.3–1.7]) children and the causes of reduced vision were undetermined in 14 (0.8% [95% CI, 0.7–2.3]) children.
The principal causes of visual impairment
The causes of UVA of 6/12 or worse at least in one eye are presented in Table 5. RE was the main cause of VI in 61 (57%) affected children. Retinal disorders (retinal degeneration and retinal detachment) were the cause of VI in 14 (13.1%) children. Amblyopia accounted for 6 (5.6%) children. Corneal opacity was the cause of vision impairment in one child (0.9%) and cataract was present in four (3.7%) children. Reduced vision was unexplained in 11 (10.3%) children and other causes of VI accounted for 10 (9.3%) children.
| TABLE 5: Causes of uncorrected visual acuity 6/12 or worse. |
Schoolchildren who received spectacles, eye drops or were referred
About 1410 (84.6%) school-aged children had normal vision and no ocular abnormalities and were not referred. The distributions of the remaining schoolchildren who received eye care or who were referred for further treatment were as follows: 216 (13.0%) schoolchildren had uncorrected RE, inflammatory and allergic eye conditions. The learners with uncorrected RE were given spectacles and the others were provided with eye drops. Forty (2.4%) learners presented with other eye diseases and were referred to an eye hospital for further treatment.
Discussion
Cycloplegic refractions were used to assess the RE of schoolchildren in this study as for previous studies by Naidoo et al.7 in South Africa as well as Pi et al.8 in China, Aldebasi25 in Saudi Arabia and Paudel et al.26 in Vietnam. The prevalence of presenting VI (UVA ≤ 6/12 in the better eye) of 4.4% is lower than 5.5% found in RESC studies by Zeidan et al.16 in Khartoum, 6.9% found by Megbelayin and Asana27 in Nigeria, 9.5% found by Mehari and Yimer28 in rural central Ethiopia and 7.7% found by Pi et al.29 in Western Chinese children aged 6–15 years. However, the prevalence from this study is higher compared to figures reported from other regions, which used the same protocol. Naidoo et al.7 in southern Africa found a prevalence of 2.1% and Salomao et al.10 in southern Latin America found a prevalence of 2.67%. However, the result of this study is similar to the prevalence of vision impairment among children in Western Africa at 4.5%.30 These results indicate that VI among school-aged children is a concern requiring urgent intervention. Thus, it is evident that lack of primary eye care to deal with childhood VI as well as lack of health education programmes to raise the awareness of the community about the consequences of childhood VI are the primary reasons for the prevalence of VI in schoolchildren. The study findings revealed no significant association between gender and prevalence of VI (p = 0.83), which was similar to studies by Megbelayin and Asana28 in Nigeria and Pi et al.29 in Western China who found no significant correlation between sex and prevalence of VI. However, our findings showed the prevalence of VI becomes higher with increasing age and grades (p = 0.00), in line with studies in Nigeria29 and Western China.29
The prevalence of RE in either eye was 178 (11.2%), which is lower than that found by school-based studies conducted in similar age groups such as those by Paudel et al.26 in Vietnam (21.4%), El Bayoumy et al.31 in Egypt (22.1%) and Al Wadaani et al.11 in Saudi Arabia (13.7%), but higher than other reports of similar age groups in Ethiopia at 9.0% by Yared et al.32 and in China at 6.3% by Li et al.33 The prevalence of RE in one or both eyes was found to increase from 6.6% in grade 2 to 12.7% in grade 8, which was statistically significant (p = 0.00).
The prevalence of RE among schoolchildren in this report was 11.2%, which is statistically significant for age and grade levels of the children (p = 0.00). However, it was lower than that reported from similar age groups in the Cape Coast of Ghana (25.6% prevalence30), Vietnam (16.3%26), Egypt (22.1%31) and Qassim Province primary schoolchildren in Saudi Arabia (at 16.3%25). However, the prevalence was higher than that found in RESC studies in South Africa at 2.4%,7 Iran at 3.5%,34 Nepal at 8.6%35 and Nigeria at 2.2%.36 On the other hand, the prevalence of RE in this study was similar to the 11.6%37 for children in Uganda as well as 13.3%30 among schoolchildren in the central region of Ghana and 13.7%25 for primary schoolchildren in Saudi Arabia. The prevalence of RE in children in the present study is also higher than that reported from other studies conducted in Africa that used the RESC protocol. A possible reason for this was that this study used the definition of RE, as per the original protocol, which defined RE’s detected when performed by cycloplegic autorefractometer.5 However, most studies conducted in African countries did not follow the RESC definition for RE and cycloplegic autorefractions were not used in the majority of the studies, except those conducted by Naidoo et al.7
The prevalence of myopia (spherical equivalent RE of −0.5 D or more in one or both eyes) was found in this study to be 6.8%, which was similar to that of 6.8%38 in Chile, 6.0%28 in Ethiopia and 5.8%25 in Qassim Province, Saudi Arabia. However, it was relatively lower than that found in Ethiopia and Ghana, where the prevalence was 13.6%32 and 14.1%30, respectively. Other studies reported a lower prevalence of myopia among school-aged children in Iran at 3.4%34 by Fotouhi et al. as well as in South Africa at 4.0%7 by Naidoo et al. and in Southern India at 4.1%39 by Dandona et al. The results of this study showed that schoolchildren in older ages and higher grades had a higher prevalence of myopia, which was similar to studies conducted in Vietnam26 and Ethiopia.32 This associated increase in the prevalence of myopia with ages and grade levels may be because of decreased outdoor activity of many children and this has been reported as an issue in other papers. This study found that there was no significant difference in the prevalence of myopia between male and female children.
The prevalence of hypermetropia in this study of 1.9% was significantly lower than that reported in other studies of similar school-aged children conducted in other countries; for instance, 26.4%32 in Ethiopia, 6.9%40 in Ghana and 9.9%11 in Saudi Arabia. However, it was similar to results found in a South African eye survey of 1.8%7 and of school-aged children in rural Northern China at 1.6%.33 Our result of a trend of increasing prevalence of hypermetropia among children with increasing age is also in line with results obtained from South Africa7 and China.32 The increase in prevalence of hypermetropia with increasing age might be because of a decrease in power of crystalline lens or loss of residual accommodation. The prevalence of hypermetropia was not significantly different between male and female children as also found, for example, by Shrestha et al.35 among Nepalese school-aged children.
The prevalence of astigmatism in the current study was 2.5%. This is much lower than the findings by Ogbomo and Assien among Ghanaian children at 6.6%30, Khalaj et al. in Iran at 16.1%41 and by Naidoo et al.7 14.6% in South Africa. However, the prevalence of astigmatism found in this study was similar to the 2.5%42 reported in Riyadh by Al-Rowaily and 2.17%28 reported in Ethiopia by Mehari and Yimer. Of the examined children, 0.3% had manifest strabismus (three children had esotropia and two had exotropia), and this was similar to findings by Wedner et al.43 among schoolchildren in rural Tanzania, where the prevalence of strabismus was 0.5%. This is lower than the 1.3% found in South African children by Naidoo et al.7 and 1.2% found among Iranian children by Jamali et al.44
In this study, uncorrected RE was the most common cause of VI among school-aged children, which accounted for 57% of cases. This result is similar to that found in many studies, which used the RESC protocol in African school-aged children such as in South Africa (66.4%7) and in Ethiopia (65.9%28). However, this result is lower than that found in Asian children at 87.3%34 reported from Iran by Fotouhi et al. and at 86.08%29 in Western China by Pi et al. These findings are lower than those in Asian children. This could be because of genetic differences as well as the different lifestyles in terms of outdoor activities of the two groups. The second cause of VI among children was retinal disorders at 13.1%, comparable to that found among South African children (10.9%7) but lower than that reported from Ethiopia (3.5%28) and Iran (0.5%34). The prevalence of amblyopia was 5.6%, which was lower than that found among Ethiopian and South African children at 9.6%28 and 9.4%7, respectively, and similar to that found in Ghana at 6.0%30. The prevalence of cataract was 3.7% relatively similar to that found in Ethiopia at 4.2%28 and South Africa at 2.3%7 by Naidoo et al. The high prevalence of the anterior- and posterior-segment abnormalities found among school-aged children in this study is a further reflection of the inadequacy of childhood eye care services in South Darfur State of Sudan.
This study revealed that the prevalence of myopia in school-aged children was slightly higher than that found in previous studies conducted among African school-aged children. However, the present study agrees with recent studies that there is a gradual increase in myopia over the last decade and this might be because of increased time spent indoors and lack of time outdoors as children are increasingly engaging in tasks using technology such as computers and mobile phones rather than outdoor activities. This trend of increasing myopia has been stated by Holden et al.,45 who reported that the prevalence of myopia worldwide was 22.9%. According to a systemic review of data from 145 studies, they predicted that this will increase to 49.8% by 2050. Our study revealed that almost two-thirds of the visually impaired children had uncorrected RE and had never received refractive correction. Naidoo et al.46 have identified that uncorrected refractive error is a major challenge globally with 108m people worldwide suffering from VI because of uncorrected RE. Our study identified this as a major public health challenge in Sudan as well. Despite the presence of significant uncorrected RE of 187 (11.2%) among school-aged children in Sudan, they did not receive RE correction, suggesting that there are significant barriers for accessing RE correction as well as lack of knowledge about the effects of uncorrected RE. Therefore, health education programmes about the use of spectacles and consequences of uncorrected RE are important as well as developing a comprehensive child eye care plan to reduce the risk of uncorrected RE.
Limitations
The current study had some limitations. Firstly, not all the schools in the South Darfur State were included in the sampling frame and the schools in the camp of internally displaced people were not included in this study. Thus, our findings reflect only the prevalence of VI and RE among school-aged children studying at public and private schools in the South Darfur State. Secondly, we conducted all the clinical eye examinations in the schools to improve the participation rate. However, conditions such as illumination, ventilation and comfort were different from school to school. However, we did ensure that we chose similar environments to conduct the study. Thirdly, the number of schoolchildren decreased in higher-grade levels, which may introduce bias in the results of VI and RE, as the numbers were not uniform across all school grades. Finally, our study employed a modified RESC protocol. This involved minor changes in the instruments that were used for collecting the data as recommended by the original protocol. We used Snellen (Tumbling E-optotype), torch and magnifier as opposed to LogMAR charts and slit lamp as well as ophthalmoscopy as opposed to fundus biomicroscopy.
Conclusion
To our knowledge, no similar study has been conducted in this region; thus, the data obtained makes a valuable contribution to the understanding of eye health challenges in the South Darfur State of Sudan. The study concluded that uncorrected RE was a major cause of VI among school-aged children in this region. These findings indicate an urgent need for developing a comprehensive childhood eye care plan for delivering eye care services to school-aged children, through collaboration between government, private sectors, stakeholders and non-government organisations working in preventing avoidable childhood blindness and VI. This supports the need for regular vision screening programmes for the prevention of avoidable causes of vision.
Acknowledgements
The African Vision Research Institute (AVRI) funded this study and we are grateful for the support of the Brien Holden Vision Institute. We thank Professor Kamal Hashim Binnawi, coordinator for prevention of blindness in Sudan, for his support and the school health promotion managers in South Darfur State Dr Jamal and Dr Adam Mousa. We also thank the data collection team for their hard work and all the students who participated in the study.
Competing interest
The authors declare that they have no financial or personal relationships, which may have inappropriately influenced them in writing this article.
Authors’ contributions
S.H.A. was the project leader who was responsible for the experimental and project design under the supervision of P.C.C-F. and K.S.N. S.H.A. conducted all clinical research. P.C.C-F. and K.S.N. made conceptual contributions and provided guidance for the study. S.H.A. was responsible for the writing of this article with input and edits from P.C.C-F. and K.S.N.
References
- Maritto SP. Global data on visual impairment 2010. Geneva: World Health Organization; 2012. WHO/NMH/PBD/.
- Naidoo KS, Jaggernath J. Uncorrected refractive errors. Indian J Ophthalmol. 2012;60(5):432–437. http://dx.doi.org/10.4103/0301-4738.100543
- Courtright P, Hutchinson A, Lewallen S. Visual impairment in children in middle- and lower-income countries. Arch Dis Child. 2011;96(12):1129–1134. http://dx.doi.org/10.1136/archdischild-2011-300093
- Alrasheed SH, Naidoo KS, Clarke-Farr PC. Childhood eye care services in South Darfur State of Sudan: Learner and parent perspectives. Afr Vision Eye Health. 2016;75(1):1–13. http://dx.doi.org/10.4102/aveh.v75i1.315
- Logan N. The development of refractive error. Optometry: Science, technique and clinical management. 2nd ed. Oxford, UK: Elsevier Health Sciences; 2009; p. 159–171.
- Resnikoff S. Assessment of the prevalence of visual impairment attributable to refractive error or other causes in schoolchildren. Geneva: National Institute of Health and WHO; 2007.
- Naidoo KS, Raghunandan A, Mashige K, et al. Refractive error and visual impairment in African children in South Africa. Durban: Invest Ophthalmol Vis Sci. 2003;44(9):3764–3770. http://dx.doi.org/10.1167/iovs.03-0283
- Pi LH, Chen L, Liu Q, et al. Refractive status and prevalence of refractive errors in suburban school-age children. Int J Med Sci. 2010;7(6):342–353. http://dx.doi.org/10.7150/ijms.7.342
- Murthy GV, Gupta SK, Ellwein LB, et al. Refractive error in children in an urban population in New Delhi. Invest Ophthalmol Vis Sci. 2002;43(3):623–631.
- Salomao SR, Cinoto RW, Berezovsky A, et al. Prevalence and causes of visual impairment in low–middle income school children in São Paulo, Brazil. Invest Ophthalmol Vis Sci. 2008;49(10):4308–4313. http://dx.doi.org/10.1167/iovs.08-2073
- Al Wadaani FA, Amin TT, Ali A, Khan AR. Prevalence and pattern of refractive errors among primary school Children in Al Hassa, Saudi Arabia. Glob J Health Sci. 2013;5(1):125–128. ISSN 1916-973.
- Naidoo KS, Wallace DB, Holden BA, Minto H, Faal HB, Dube P. The challenge of uncorrected refractive error: Driving the agenda of the Durban Declaration on refractive error and service development. Clin Exp Optometry. 2010;93(3):131–136. http://dx.doi.org/10.1111/j.1444-0938.2010.00455.x
- Holden BA. Uncorrected refractive error: The major and most easily avoidable cause of vision loss. Community Eye Health. 2007;20(63):37–39.
- World Health Organization. Saving the lives of the mother and children. Rising to the challenge. Khartoum: WHO; 2013. WRH/WP/13.16.
- Kassak KM. Knowledge, attitudes and practice (KAP) in Sudanese communities for their health seeking behavior. Khartoum: Federal Ministry of Health; 2011.
- Zeidan Z, Hashim K, Muhit MA, Gilbert C. Prevalence and causes of childhood blindness in camps for displaced persons in Khartoum: Results of a household survey. East Mediterranean Health J. 2007;3(13):580–585.
- Binnawi KH. Progress in blindness prevention in North Sudan (2003–2010). Sudanese J Ophthalmol. 2013;5(1):3. http://dx.doi.org/10.4103/1858-540X.118638
- Kim G, Torbay R, Lawry L. Basic health, women’s health, and mental health among internally displaced persons in Nyala Province, South Darfur, Sudan. Am J Public Health. 2007;97(2):353–361. http://dx.doi.org/10.2105/AJPH.2005.073635
- Ismail KA, Khlafala H. Householders and housing characteristics 5th Population Census 2008. Khartoum: Central Bureau of Statistics Census; 2008.
- Sudan Central Bureau of Statistics. Sudan National Baseline. Sudan Household Survey 2009 North Sudan. Khartoum: Central Bureau of Statistics (CBS); 2009.
- Ministry of Education South Darfur State. An overall number of students enrolment in primary school of South Darfur in 2014–2015. Nyala: Ministry of Education; 2015.
- Logan N. The development of refractive error. In optometry science, technique and clinical management. Landon: Butterworth-Heinemann; 2009.
- Muma MK, Kimani K, Kariuk, Wanyike MM. Prevalence and significant refractive errors in primary school children of a rural district of Kenya. East Afr J Ophthalmol. 2007;13(2):48–51.
- Minassian D. Epidemiology in practice: Sample size calculation for eye surveys: A simple method. Community Eye Health. 1997;10(23):42–44.
- Aldebasi HY. Prevalence of correctable visual impairment in primary school children in Qassim Province. J Optometry. 2014;7(3):168–176. http://dx.doi.org/1016/j.optom.2014.001
- Paudel P, Ramson P, Naduvilath T, et al. Prevalence of vision impairment and refractive error in schoolchildren in Ba Ria – Vung Tau province, Vietnam. Clin Exp Ophthalmol. 2014;42(2):217–226. http://dx.doi.org/10.1111/ceo.12273
- Megbelayin O, Asana E. Visual impairment among schoolchildren calabar vision screening survey in secondary schools (CVS4 Study). The Internet J Ophthalmol Vis Sci. 2013;10(1):1–7.
- Mehari ZA, Yimer AW. Prevalence of refractive errors among schoolchildren in rural central Ethiopia. Clin Exp Optom. 2013;96(1):65–69. http://dx.doi.org/10.1111/j.1444-0938.2012.00762.x
- Pi LH, et al. Prevalence of eye diseases and causes of visual impairment in school-aged children in Western China. J Epidemiol. 2012;22(1):37–44. http://dx.doi.org/10.2188/jea.JE20110063
- Ovenseri-Ogbomo GO, Assien R. Refractive error in schoolchildren in Agona Swedru, Ghana. Afr Vis Eye Health. 2010;69(2):86–92.
- El-Bayoumy BM, Saad AA, Choudhury H. Prevalence of refractive error and low vision among schoolchildren in Cairo. East Mediterranean Health J. 2007;13(3):1575–1579.
- Yared AW, Belaynew WT, Destaye S, Ayanaw T, Zelalem E. Prevalence of refractive errors among school children in Gondar town, northwest Ethiopia. Middle East Afr J Ophthalmol. 2012;19(4):372–376. http://dx.doi.org/10.4103/0974-9233.102742
- Li Z, Xu K, Wu S, Lv J, Jin D, Song Z, Wang Z, Liu P. Population-based survey of refractive error among school-aged children in rural northern China; the Heilongjiang eye study. Clin Exp Ophthalmol. 2014;42(4):379–384. http://dx.doi.org/10.1111/ceo.12198
- Fotouhi A, Hashemi H, Khabazkhoob M, Mohammad K. The prevalence of refractive errors among schoolchildren in Dezful, Iran. Br J Ophthalmol. 2007;91(3):287–292. http://dx.doi.org/10.1136/bjo.2006.099937
- Shrestha GS, Sujakhu D, Joshi P. Refractive error among school children in Jhapa, Nepal. J Optom. 2011;4(2):49–55. http://dx.doi.org/10.1016/S1888-4296(11)70041-3
- Opubiri I, Pedro-Egbe CN. Screening of primary school children for refractive error in South-South Nigeria. Ethiop J Health Sci. 2012;22(2):129–134.
- Kawuma M, Mayeku R. A survey of the prevalence of refractive errors among children in lower primary schools in Kampala district. Afr Health Sci. 2002;2(2):69–72.
- Maul E, Barroso S, Munoz S, Sperduto R, Ellwein L. Refractive error study in children: Results from La Florida, Chile. Am J Ophthalmol. 2000;129(4):445–454. http://dx.doi.org/10.1016/S0002-9394(99)00454-7
- Dandona R, Dandona L, Srinivas M, et al. Refractive error in children in a rural population in India. Invest Ophthalmol Vis Sci. 2002;43(3):615–622.
- Ovenseri-Ogbomo GO, Omuemu VO. Prevalence of refractive error among school children in the Cape Coast Municipality, Ghana. Clin Optom. 2010;2:59–66. http://dx.doi.org/10.2147/OPTO.S10583
- Khalaj M, Gasemi M, Zeidi IM. Prevalence of refractive errors in primary school children [7–15 years] of Qazvin City. Eur J Sci Res. 2009;28(2):174–185. ISSNN1450-216X.
- Al-Rowaily MA. Prevalence of refractive errors among pre-school children at King Abdul-Aziz Medical City, Riyadh, Saudi Arabia. Saudi J Ophthalmol. 2010;24(2):45–48. http://dx.doi.org/10.1016/j.sjopt.2010.01.001
- Wedner SH, Ross DA, Balira R, Kaji L, Foster A. Prevalence of eye diseases in primary school children in a rural area of Tanzania. Br J Ophthalmol. 2000;84(11):1291–1297. http://dx.doi.org/10.1136/bjo.84.11.1291
- Jamali P, Fotouhi A, Hashemi H, Younesian M, Jafari A. Refractive errors and amblyopia in children entering school: Shahrood, Iran. Optom Vis Sci. 2009;86(4):364–369. http://dx.doi.org/1040-5488/09/8604-0364/0
- Holden BA, Fricke TR, Wilson DA, et al. Global prevalence of Myopia and High Myopia and temporal trends from 2000 through 2050. Ophthalmology. 2016;123(5):1036–1042. http://dx.doi.org/10.1016/j.ophtha.2016.01.006
- Naidoo KS, Leasher J, Bourne RR, et al. Global vision impairment and blindness due to uncorrected refractive error, 1990–2010. Optom Vis Sci. 2016;93(3):227–234. http://dx.doi.org/10.1097/OPX.0000000000000796
|



